The development and duration of immunity to SARS-CoV-2 following infection or vaccination is not fully understood, but increased knowledge is crucial for the vaccination drive against COVID-19. A trio of new assays for quantitative measurement of IgG antibodies against the viral spike protein domain S1 including the receptor-binding domain (RBD), detection of neutralising antibodies targeting S1/RBD, and determination of SARS-CoV-2-reactive T cells supports the differentiated investigation of SARS-CoV-2-specific immune responses. This comprehensive analysis is especially useful for studying vaccine responses with the goal of optimising vaccination strategies.
Immune responses to SARS-CoV-2
Both humoral and cellular components of the immune system are involved in building immunity against SARS-CoV-2 and providing protection against reinfection with the virus. Antibodies of class IgG against the S1/RBD of the viral spike protein and specific long-lived T cells are suspected to play the most relevant roles in virus neutralisation and sustained immunity.
The immunodominant RBD of the S1 subunit is responsible for binding to the human cellular receptor angiotensin-converting enzyme 2 (ACE2) and mediating entry of the virus into the host cells. Specific antibodies from previous infection or vaccination can block the RBD and prevent the virus from invading the host cells. However, it is currently not known what level of antibodies confer protection against COVID-19 or how long the immune protection lasts. Establishing the correlate of protection, that is the concentration of antibodies at which immunity can be assumed, requires large-scale studies and long-term observations and is usually determined by an evidence-based approach. The quantitative determination of antibody concentrations in patients and vaccinated individuals provides valuable support in clarifying this threshold. Measurement of the neutralising activity of these antibodies is also important for confirming the functionality of the antibodies, namely their ability to inhibit S1/RBD binding to ACE2 and prevent infection. Neutralising antibodies can generally be determined 14 to 21 days after infection or vaccination.
T-cell immunity, particularly to the spike protein, appears to be associated with strong protection, even in patients who do not exhibit detectable levels of antibodies. According to current knowledge, about 10 per cent of symptomatic and 40 per cent of asymptomatic patients lose their IgG antibodies, so that a past infection or response to vaccination may only be detectable via the T-cell response. Therefore, the measurement of specific T-cell responses is an additional important tool for studies into SARS-CoV-2 immunity and vaccine efficacy.
As of March 2021, the World Health Organisation (WHO) and the London School of Hygiene and Tropical Medicine have documented more than 310 COVID-19 vaccine candidates, of which 87 have reached clinical trials and several are now authorised for use in various countries. The different vaccine approaches include vaccines based on mRNA, DNA, viral vectors, protein subunits, inactivated virus, virus-like particles or live attenuated virus. The spike protein constitutes the main target for COVID-19 vaccines.
Quantitative anti-S1 antibody detection
In December 2020, the WHO approved the first international reference material for the standardisation of results from anti-SARS-CoV-2 serological assays (First WHO International Standard for anti-SARS-CoV-2 immunoglobulin, NIBSC code: 20/136). This enables antibody concentrations to be measured reliably in standardised units and harmonised between test systems. As a participant in the characterisation of this reference serum, EUROIMMUN was able to rapidly align its quantitative S1-based ELISA to this standard. The new CE-marked and fully automatable Anti-SARS-CoV-2 QuantiVac ELISA (IgG) is one of the first commercial antibody tests to provide quantification of the antibody concentration in standardised units (binding antibody units, BAU/ml). The assay uses a 6-point calibration curve. The quantitative ELISA was tested using serial dilutions of the WHO reference serum (Figure 1) and yielded an excellent correlation with the standard (coefficient of determination r2 = 0.99).
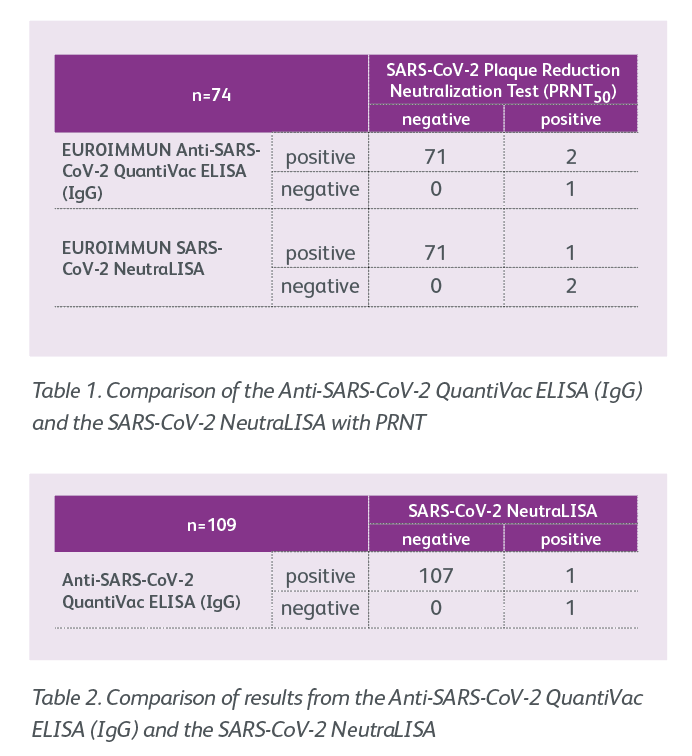
The S1 antigen is the least evolutionarily conserved within the coronavirus family, therefore antibodies against it are very specific for SARS-CoV-2. The Anti-SARS-CoV-2 QuantiVac ELISA (IgG) exhibits a specificity of 99.8 per cent, as demonstrated in a large cohort including sera positive for antibodies against other human pathogenic coronaviruses or other infectious agents as well as sera from healthy blood donors collected prior to 2020 (n=1458). As the S1/RBD antigen is the main target for virus neutralisation, the antibodies detected with this ELISA are with high likelihood neutralising antibodies. To verify this, the ELISA was compared with a plaque reduction neutralisation test (PRNT) using 74 samples from patients with a past confirmed SARS-CoV-2 infection. There was a 97.3 per cent agreement between results from the ELISA and the PRNT (Table 1), confirming that the ELISA detected neutralising antibodies in all but three of the samples.

Correlation of the Anti-SARS-CoV-2 QuantiVac ELISA (IgG) with the WHO standard
Determination of neutralising antibodies
The PRNT or virus neutralisation test (V-NT) represents the gold standard for determining neutralising antibodies but is time-consuming and expensive to perform and requires biosafety level 3 (BSL-3) laboratory conditions due the use of pathogenic virus. A new CE-marked ELISA provides fast and economical determination of the inhibiting effect of anti-SARS-CoV-2 antibodies. The SARS-CoV-2 NeutraLISA is based on a competitive principle, whereby neutralising antibodies in the patient sample compete with added biotinylated ACE2 receptors to attach to the binding sites of recombinant S1 antigen coated onto the microplate wells. The results are evaluated qualitatively as positive/negative using a cut-off of 25 per cent inhibition. The ELISA is linear in the range up to 67 per cent inhibition and shows an excellent correlation with the WHO international reference standard in this range (coefficient of determination r2 = 0.98). The cut-off area of the test corresponds to a value of around 62 IU/ml. The specificity of the ELISA amounted to 99.7 per cent in a cohort including sera positive for antibodies against other human pathogenic coronaviruses or other infectious agents, sera with a negative result in a SARS-CoV-2 neutralisation test and sera from healthy blood donors taken prior to 2020 (n=759).
The performance of the SARS-CoV-2 NeutraLISA for detecting neutralising antibodies was investigated by comparing the assay with a PRNT in 74 samples from patients with a past confirmed SARS-CoV-2 infection. There was a 98.6 per cent agreement of qualitative results between the two tests (Table 1). The ELISA offers the advantage of being much quicker to perform than the PRNT, with results being available within two hours rather than days. Moreover, it does not require BSL-3 conditions and is therefore suitable for routine laboratory diagnostics. The assay can be fully automated, for example on the EUROIMMUN Analyzer I or I-2P or the EUROLabWorkstation ELISA, making it ideal for use in a high-throughput capacity.
Results from the SARS-CoV-2 NeutraLISA were additionally compared with those from the Anti-SARS-CoV-2 QuantiVac ELISA (IgG). In the tested cohort there was a 99.1 per cent agreement between the qualitative results (Table 2, borderline results excluded). In isolated cases, results from the neutralisation test and quantitative anti-S1 IgG determination may be discrepant. Possible reasons include the presence of high concentrations of IgA antibodies with an inhibiting function, which are detected in addition to IgG by the neutralisation test, but not by the Anti-SARS-CoV-2 QuantiVac ELISA. In these cases, it may be helpful to repeat the investigations 7 to 14 days later.
Analysis of specific T-cell responses
Cellular immunity to SARS-CoV-2 conferred by long-lasting T cells can be measured using the SARS-CoV-2 Interferon-Gamma Release Assay (IGRA). Interferon-gamma is an important signalling molecule of the immune system which is released by the T cells upon contact with the virus. The IGRA is performed on heparinised whole blood samples, circumventing the need to prepare purified peripheral blood mononuclear cells (PBMCs). The T cells in the patient blood samples are stimulated based on specific viral spike protein in the provided tubes. The interferon-gamma released by the T cells is subsequently determined using a fully automated quantitative ELISA. The IGRA is a particularly useful tool for studies investigating the cellular immune response in SARS-CoV-2 infected or vaccinated individuals. The EUROIMMUN assay is currently available for research use only.
Perspectives
Vaccines against SARS-CoV-2 constitute the most important arsenal for combatting the COVID-19 pandemic. The first authorised vaccines are now being applied worldwide and a myriad of further candidates are in development and clinical trial phases. The ideal vaccine induces high titers of neutralising antibodies as well as robust T-cell responses. A comprehensive evaluation of the different arms of the immune response is therefore critical for assessing vaccine responses. Establishing immune correlates of protection will aid, in particular, the rapid assessment of future vaccine candidates and the fine-tuning of immunisation strategies with regard to dosage and timing of boosters. The durability of immunological memory and cross-protection between SARS-CoV-2 variants will also remain a major focus of research. Analysing both antibody and T-cell immunity additionally facilitates long-term epidemiological surveillance, especially for modelling population-level immunity.
This article appears in the latest issue of Omnia Health Magazine. Read the full issue online today, covering femtech, AI, IoT and much more.