We value gold, and we, therefore, transport it and secure it with very high levels of care. When we think of gold being moved, we imagine a specialist, hopefully, an impregnable security truck making sure that every single ounce of this precious substance is delivered.
But, in comparison to many medications routinely given in oncology regimens and in auto-immune therapies, gold is cheap. Gold’s value hardly equates in value to many of the new generation Monoclonal Antibodies and Gene Therapies, either by ‘per ounce’ value or in its societal value and, of course, in its value to the patient. Furthermore, the price of gold has in fact declined by 9.1 per cent in the last 10 years whilst total pharmaceutical expenditure in member countries of the Organization for Economic Cooperation and Development (OECD) has increased by some 30.1 per cent despite overall consumption only increasing by 7.1 per cent in the same period. (Figure 1)

Figure 1. Medication Price Changes vs. Gold Prices 2010-2018.
This has triggered many healthcare providers to consider economic arrangements where the financial impact attached to the introduction of new therapies is shared between the payer and the medication’s manufacturers in so-called risk-sharing agreements or outcomes-based contracts. This is certainly laudable and follows a fundamental rule of Value-Based Healthcare; to make the most effective and efficient allocation of scarce resources to meet specified goals.
This said once we have these medications available to us, the second rule of Value-Based Healthcare is to obtain the maximum cost-benefit from the treatments and strategies we employ for patient care. This is where technology, speciality materials and education and training of staff enters the arena.
It is logical that these medications with a monetary value far exceeding that of gold should be as carefully and securely stored as any other precious item. This is an area that technology has already had an impact on the management of Controlled Substances. Central pharmacy integrated medication safes that store, track, and monitor the location and withdrawal of narcotics from satellite Automated Dispensing Cabinets and Anaesthesia Stations can also store high-value medications to reduce the risk of their loss or diversion. This kind of set-up can easily also securely accommodate high-value medications (including intravenous products prior to reconstitution) at every part of their journey from central through to served areas to provide seamlessly, facility-wide management of ‘precious’ inventory.
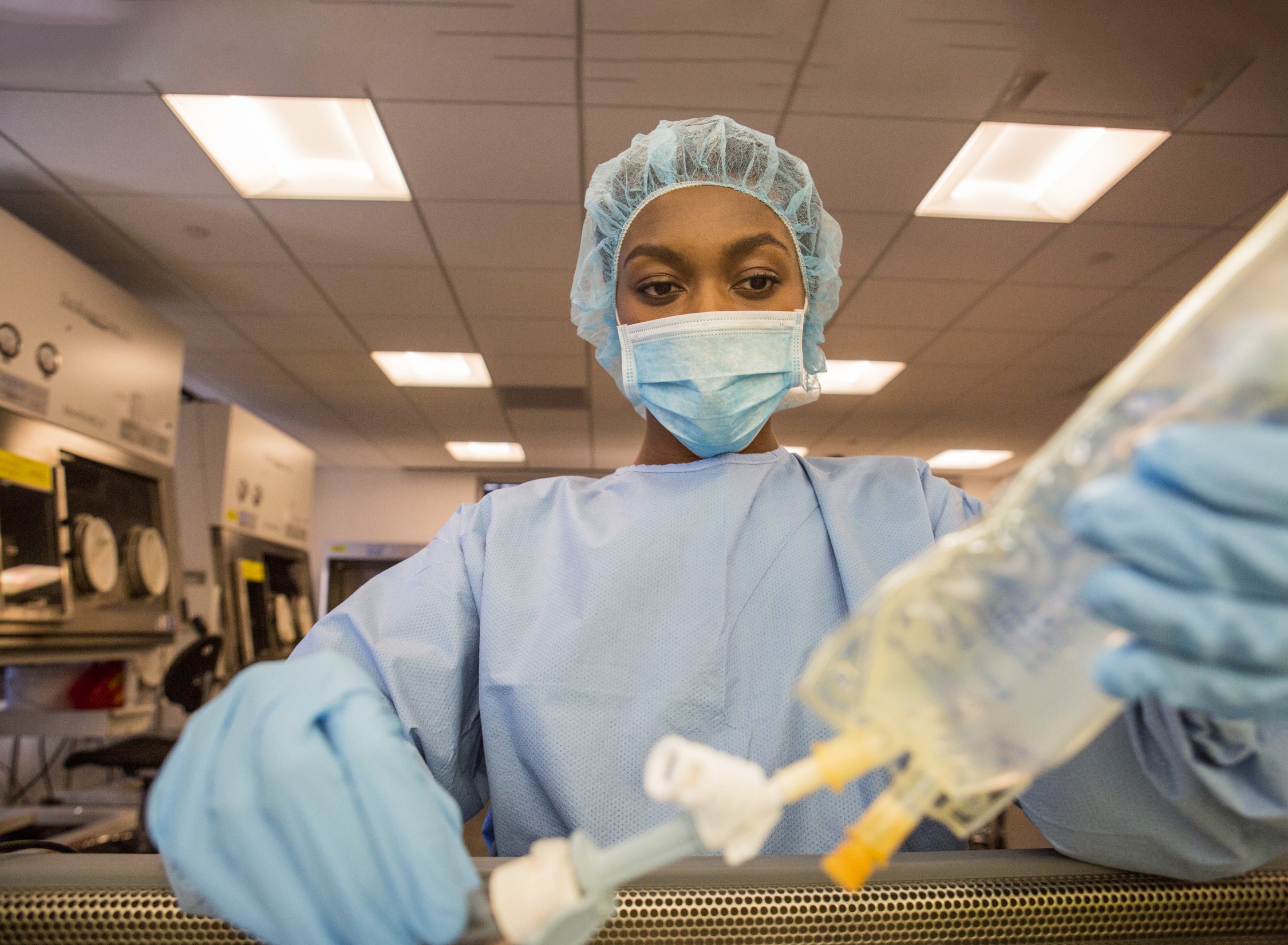
Gravimetric compounding systems can record preparation steps and track high-value medications through to patient administration.
Reconstitution of high-value oncology medications is a key process as the potential for hugely expensive wastage through incorrect compounding is a consistent risk. Pharmacist-led double-checks of the technicians’ compounding is difficult to manage as the IV prep clean-room is a deliberately isolated environment. Advanced pharmacy systems that allow for remote checking of correct compounding, and which use barcode scanners to check the correct drug for compounding against the electronic prescription, to deliver appropriate manufacturers’ warnings and precautionary advice as a ‘recipe’ for the technician to follow and employ gravimetric systems for dose/dilution checking help reduce this risk significantly. The entire compounding process can be recorded for checking and record-keeping by automated digital photographic capture of all key stages of compounding and of the final product. This technology allows the pharmacist to be outside of the cleanroom, but in-fact maintain a greater oversight of dosing/dilution than is possible with intermittent checks only being made at critical preparation points.

Many high-value medications require speciality IV administration lines.
The final printed barcode label for high-value chemotherapy created through an advanced compounding solution allows for tracking through connected inventory systems. Storage of the reconstituted product may require temperature control and light-protection. This is best achieved through medical-grade ‘intelligent’ refrigerators that are also integrated into the medication tracking and inventory system and which have distinct secure compartments within.
The reconstituted high-value medication’s barcode label must also include patient details, drug dose and volume and should also include vitally important instructions for administration, including precautions in terms of the IV administration line required for safe, effective and uncorrupted delivery of this high-value and vital medication to the patient.
It is a common misconception that all IV administration lines are the same. They are not. Incorrect administration line selection by the clinician can cause deleterious changes to the active ingredients in the high-value medication being given. Not only is this potentially harmful to the patient as chemical change may take place in the medication upon contact and interaction with administration line material (the creation of peroxides when some medications and parental nutrition products are exposed to light during administration is an example of this) but there may also be a significant loss in the efficacy of the medication and a degrading of its therapeutic value. Not only is this equivalent to incorrect administration of the medication, it is also potentially a waste of the full monetary value of the medication (a medication that we have purchased at a cost greater than that of gold!)
A good example of the absolute need for the correct selection of administration line for a particular medication is that of the Taxol group of chemotherapeutic medications. These medications require low-sorbing lines and 0.2-micron filtration. The most suitable line for these medications is one with an inert polyethylene lined inner surface which does not allow the medication to come into contact with the PVC body of the line and thus avoids the risk of PVC-plasticizers leaching out from the administration line and into the medication, and with an integrated filter close to the patient.
For IV administration of most Monoclonal Antibodies (such as Daratumumab) an in-line, sterile, non-pyrogenic, low protein-binding polyethersulfone (PES) 0.2-micron filter is required.

High-value medications can be tracked and secured via integrated, controlled entry systems right from the central pharmacy through to patient administration.
Another issue for the giving of all chemotherapy regimens, and one which has a particular resonance with high-value medications especially for paediatric oncology, is ensuring ‘complete dose’. Running infusions down to completely empty the IV administration tubing of the medication can be difficult to manage in a busy oncology ward or outpatient unit, where one nurse is managing several patients. There are several possible solutions for this issue.
So-called ‘short sets’ that allow independent IV channel rate-control over infusions added to primary infusions of maintenance or hydration fluids. A double-channel or multi-channel pump is ideal for this technique.
Solutions at the spike-level of the administration set with self-sealing connections that allow the clinician to ‘unlock’ from a primary bag, ‘lock’ to the medication to be given, complete the infusions and run the medication bag dry whilst avoiding entry of any air into the administration line due to the IV drip chamber being below the lock-unlock unit, and then returning to the main crystalloid infusion being used for primary line flushing and patient hydration. The same lock-unblock unit allows for switching between several different medications during complex regimens.
Microbore sets that minimise the volume of medication left in the tubing, these sets can have residual volumes as small as 6 millilitres and can be cleared with small flushes.
Beyond oncology, up-to-date and comprehensive IV medication compatibility tables are increasingly difficult to source as multiple new products enter the pharmaceutical market each year. Medication incompatibilities have been suggested as a reason for the failure of both peripheral and central venous access catheters in recent studies, and recommendations on the employment of in-line filtering (either 1.2 micron or 0.2 micron, dependent on the medication/fluid being administered) have been given by study authors. Again, this is essentially a patient safety and quality issue but also carries an economic cost, particularly in the case of unscheduled replacement of central or PICC lines.
One common area of confusion for high-value medications, and also for more ‘general use’ IV medications, is the question of light-protection of infusions. A simple example of this is that a medication such as Epinephrine/Adrenaline which has photostability when mixed in Normal Saline, but which becomes photolabile when mixed in Dextrose solutions.
Pharmaceutical manufacturers give guidance on the protection of their products from light exposure during storage and transport, but advice on protection during administration is more difficult to find. Clinicians will, in fact, find more comprehensive information on this subject, and on all the other areas covered here, via the Clinical and Medical Affairs offices of medication management, infusion pump, and disposables manufacturers. Some common examples of the need for speciality lines in oncology regimens are given in Table 1.
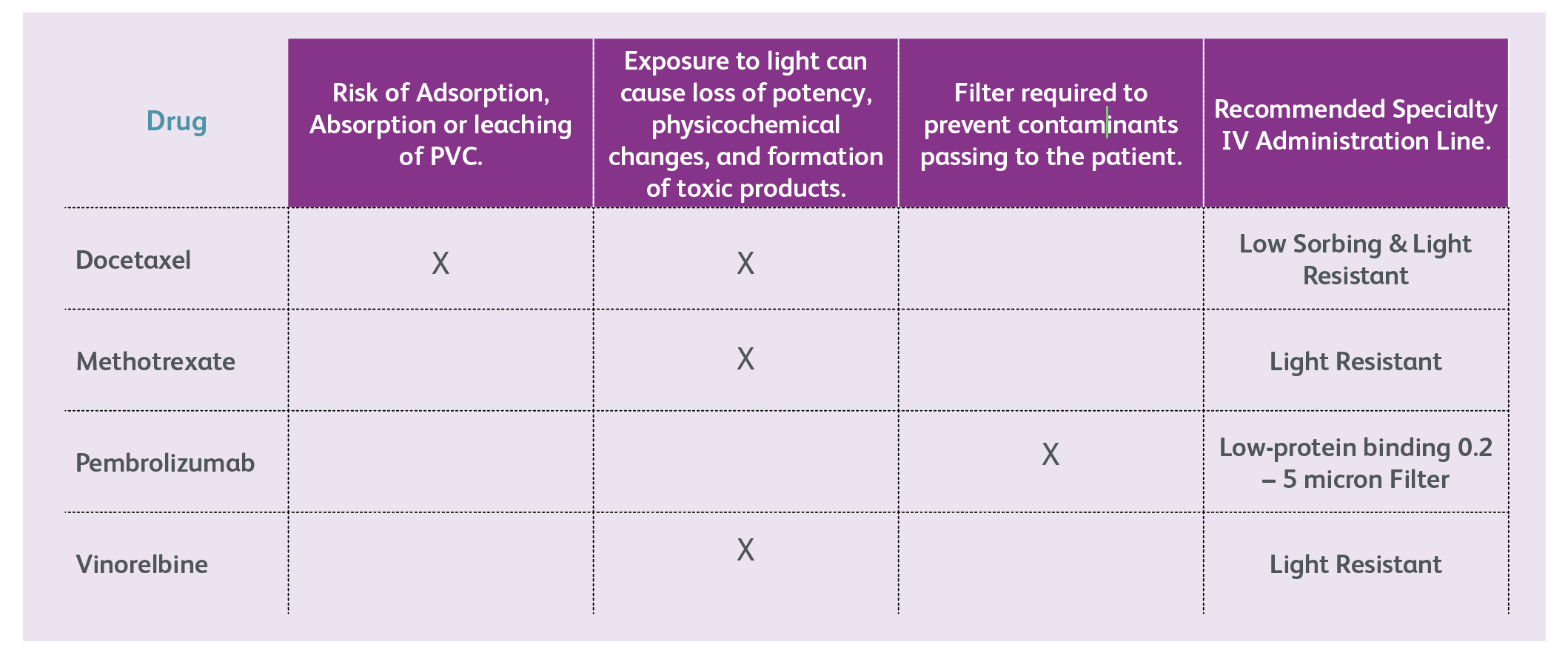
Table 1: Examples of Chemotherapy Agents and Requirements for Specialty IV Administration Lines.
When compared to the cost of even common medications, and in particular to the cost of newly patented high-value medications and to the waste and detriment to quality care that can occur through incorrect storage, tracking, compounding and administration of intravenous medications the Return on Investment from managing and administering these medications with the care that we should naturally give to such precious and expensive items is undoubtedly significant.
This article appears in the latest issue of Omnia Health Magazine. Read the full issue online today, covering cybersecurity in healthcare, the ongoing rise of telehealth and much more.


