Quick links:
Friday 26 June 2020
9.06pm
And that’s a wrap. It’s been a busy and, to use a well worn word now, unprecedented week. Lots to take in - one of the more prevalent messages coming out of the week's sessions is that we all need to work better together - public, private, countries, institutions, society.
Thanks to everyone who made Omnia Health Live a success, and let’s keep the conversation going.
8.51pm
An interesting, wide-ranging discussion is happening now on health system recovery after COVID-19 - topics mentioned include AI, telemedicine, politics, and equitable health outcomes.
8.38pm
Earlier this evening experts came together to discuss vaccinations at risk in a session moderated by Mexico-based Dr Rodrigo Romero Feregrino. Points included the following:
- Dr Alfonso Rodriguez Morales warned of the COVID-19 cases in Colombia coming from Venezuela in what he described as a complex problem - an epidemic upon previous epidemics, which has impacted health systems across the region.
- Dr Pablo Kuri agreed that owing to lack of coverage in Venezuela, measles has been reintroduced across the continent, and warns of a great risk of other diseases re-emerging. He added that COVID-19 has “kidnapped” the health agenda; and while a good treatment or vaccine doesn’t exist yet for coronavirus, other vaccinations in countries must not be overlooked.
- MSF's Barbara Saitta shared an Africa perspective, pointing to a WHO/Unicef survey of 107 countries that showed major disruption to immunisation activities on the continent, saying that an 8-10% in immunisation coverage over the last 2-3 months has meant tens of thousands of children not receiving vaccinations.
- From Chile, Dr Jan Paul Wilhelm stressed the need to continue vaccinating and this message needs to be disseminated to the public, focusing on pregnant women, children under 2 years and diseases like measles and flu.
The panel also discussed trust, learnings from earlier outbreaks in Africa, and how people can overcome the fear of receiving vaccinations, among other focus areas. We'll bring a full article to you soon!
6:45pm
At the ‘Healthcare Investment Panel’ this evening, panellist Dr Helmut Schuehsler, Chairman and CEO, TVM Capital Healthcare said that the fear factor is severely hitting healthcare companies.
“One of the first challenges of COVID-19 has been to separate fact from fiction,” he said. “One of our investments in home healthcare was hit quite hard and it's surprising because in a pandemic situation you would assume these services would come to the rescue. But because of mass hysteria created by people, patients were scared to let nurses and doctors in their homes. But we are hopeful it will pick up in the coming months.”
Schuehsler also shared that one of their IVF clinics lost 70 per cent of its business and is slowly picking up. One of the other issues has been convincing patients they are safe when they come to the hospital as well as convincing healthcare professionals that they will be provided with a safe environment to work in. Disruption in the supply chain has also become a big problem.
While Sunil Thakur, Managing Director, Quadria Capital, said that due to COVID-19, in India there was regulatory chaos, elective surgeries stopped, and due to such elements, healthcare delivery suffered. The pharma industry suffered as well due to broken supply chain, but came back within a few weeks and has been doing well since.
For Supreet Manchanda, Managing Director, Raiven Capital, the matter of building trust in this new environment is a key concern. “We have been discerning through the fake stuff. Everybody was peddling Coronavirus cures. Individually we can make fun of it but in totality it creates paralysis. On the start-up side, we have to create a level of trust on a video call. We have to re-engineer the trust factor from the start. How do you move your business forward? That is creating a dissonance. Who survives and who succeeds?”
Furthermore, he stressed that companies need to become digital otherwise they won’t survive. “We are now facing cybersecurity issues in healthcare. We are having to put security regulations on pacemakers! New companies will have to come in and rethink current business models.”
4:35pm
As part of the CME-accredited panel discussion, ‘Future surgery: which technologies will make the biggest impact?’, Dr Stanley W. Ashley, Senior Surgeon at Brigham and Women's Hospital and Frank Sawyer Professor of Surgery at Harvard Medical School, shared that Brigham’s had shut down all elective surgeries from the end of March.
“During that time, we had a steady flow of 150-200 COVID-19 patients at any given point,” he said. “At that time, we really just did emergency operations and many of our surgeons were deployed to other roles such as in the ICU. About three weeks ago, we began to open up and steadily increased the operating rooms that were running, but it has been mostly urgent cases and those with cancer with a specific timeline. This week, we will be resuming elective surgeries.”
The surgeon shared that the hospital has been seeing all outpatients virtually and that has made a big difference. “I doubt we will go back to seeing as many patients in person in the future,” he added.
While Prof Tim Pawlik, Chair of Surgery, Ohio State University Wexner Medical Center, shared that previously at the hospital, they were doing fewer than a 100 telemedicine visits but today they are conducting almost 14,000 of these a month, both telephonic and tele-video. “This has revolutionised how we are interacting with our patients. And I too am of the opinion that many of the patients will continue to prefer these virtual visits,” he said.
However, Prof Pawlik shared that this has raised a couple of issues such as how can hospitals maintain the experience and educational experience of their trainees. The other challenge has been that there are some individuals who might not have access to broadband Internet, especially those who are of a lower economic socio status. “We have to be cognizant about how we roll out telemedicine and telehealth relative to certain social determinants of health,” he stressed.
4pm
Happy mid-afternoon!
Wouter Molman, Executive Vice President Healthcare, Informa Markets, has shared a video message in which he offers thanks "for the overwhelming positive and encouraging feedback you have given us.", as well as news of upcoming events:
2:45pm
At this afternoon’s ‘Antibody-associated autoimmune encephalitis: an overview’ session presented by EUROIMMUN, Dr Romana Höftberger, a neuropathologist at the Medical University of Vienna, discussed paraneoplastic and autoimmune encephalitis with autoantibodies to intracellular or neuronal surface proteins. It induces characteristic clinical syndromes such as limbic, multifocal or diffuse encephalitis.
While classic paraneoplastic syndromes most likely result from a T cell response and intracellular antibodies are considered as an epiphenomenon, there is strong evidence that surface antibodies mediate defective synaptic signalling by interfering with the targeted antigen.
She said: “The antibody-associated autoimmune encephalitis disease can be divided into several sub-groups. First one is autoimmunity with antibodies against intracellular neuronal antigens, second is autoimmunity with antibodies against neuronal surface antigens and third is autoimmunity with antibodies against glial antigens. The fourth group is encephalitis without detectable antibodies.”
Dr Höftberger shared antibody test methods and went on to describe potential pitfalls and limitations.
1.28pm
Our own Peter Hall's mental health talk arrived at the right time on Day 5 of a hyperbusy week. Short, but sweet, his message focused on the 'Triangle of Happiness', a concept he learned at Cranfield, of maintaining family, work and oneself in equilibrium to achieve happiness. One line in particular resonated personally: "Life is a marathon, not a sprint". Pace yourselves. Trust the triangle.
12:50pm
At the ‘Operating through the endoscope: The new minimally invasive surgery revolution’ panel discussion, all the panellists agreed that COVID-19 has posed significant challenges to the practice of endoscopy.
They said that on one hand the virus could be transmitted through the GI tract and the other thing is that the procedure produces aerosolization and the challenge is how to protect staff and patients and provide endoscopic services in a safe and effective manner.
Prof Dr Barham Abu Dayyeh, Director of Advanced Endoscopy, Rochester, Minnesota, U.S., said: “Our efforts have been focused into three buckets. The first is pre-procedural testing, the second is social distancing practice and the third is aerosol mitigation.”
11:55am
New York City was the epicentre of the Coronavirus in the U.S. and witnessed a very high hospitalisation rate of COVID-19 patients. According to Dr Paul Frisch, Chief of Biomedical Physics and Engineering, Memorial Sloan Kettering Cancer Center, New York City, 22 per cent of the patients that showed required ICU level care while 79 per cent of ICU patients required ventilation.
Speaking at the ‘COVID-19 insights and lessons learnt from New York’ session, Dr Frisch said the pandemic stretched the operations of hospitals quite a bit.
He said: “At our hospital, we have a 3D printing laboratory running six printers. During the crisis, there were certain things that came up in the design and development. We had a feeling that there would be a shortage of ventilators and supplies such as nasal swabs, N95 masks, and we had to address that in a variety of ways.”
To ensure there was continuous supply, the hospital built a simple intubation-extubation device that was placed over the patient and enabled doctors to perform intubation and extubation without worrying about splatter and reduced exposure of patients. They also built the ventilator octopus, which is patented and ran it through the FDA. It enables to vent multiple patients on a single vent and each patient’s actual ventilation can be regulated independently and became a critical support device.
Moreover, they built a variety of scuba shields and masks, which were requested by anaesthetists and made modifications to face masks to enable a variety of filtering methods to be used on a single mask. Additionally, the hospital produced 3D printed nasal swabs as back-up, which were evaluated by the clinical laboratories and ran clinical trials on it to ensure its efficiency.
“I saw COVID-19 as a great demonstration of what biomedical engineering can contribute to hospital operations all over the world,” he added.
10:50am
The main goal for any disaster situation is that healthcare institutions need to maintain victim flow management, said Dr Nisreen Maghraby, EM/Trauma & Disaster Management Consultant, Chairperson Emergency & Disaster Preparedness Unit & Chairperson, KSA.
Speaking at this morning’s ‘Emergency preparedness & top tips for emergency medicine practitioners and pre-hospital care professionals’ panel discussion, she highlighted that one of the most important considerations in a pandemic is external communication.
“It is important to have bi-directional communication between your institution and other bodies in the region,” she said. “You as a healthcare institution should communicate by sending situational reports to your regional disaster centres or other hospitals. You also have to get back information about how other hospitals are functioning and what their status is. That will help in adapting the model and adjusting according to what’s happening around you.”
Dr Maghraby also shared the below diagram about the layers of pressures being faced by healthcare institutions.
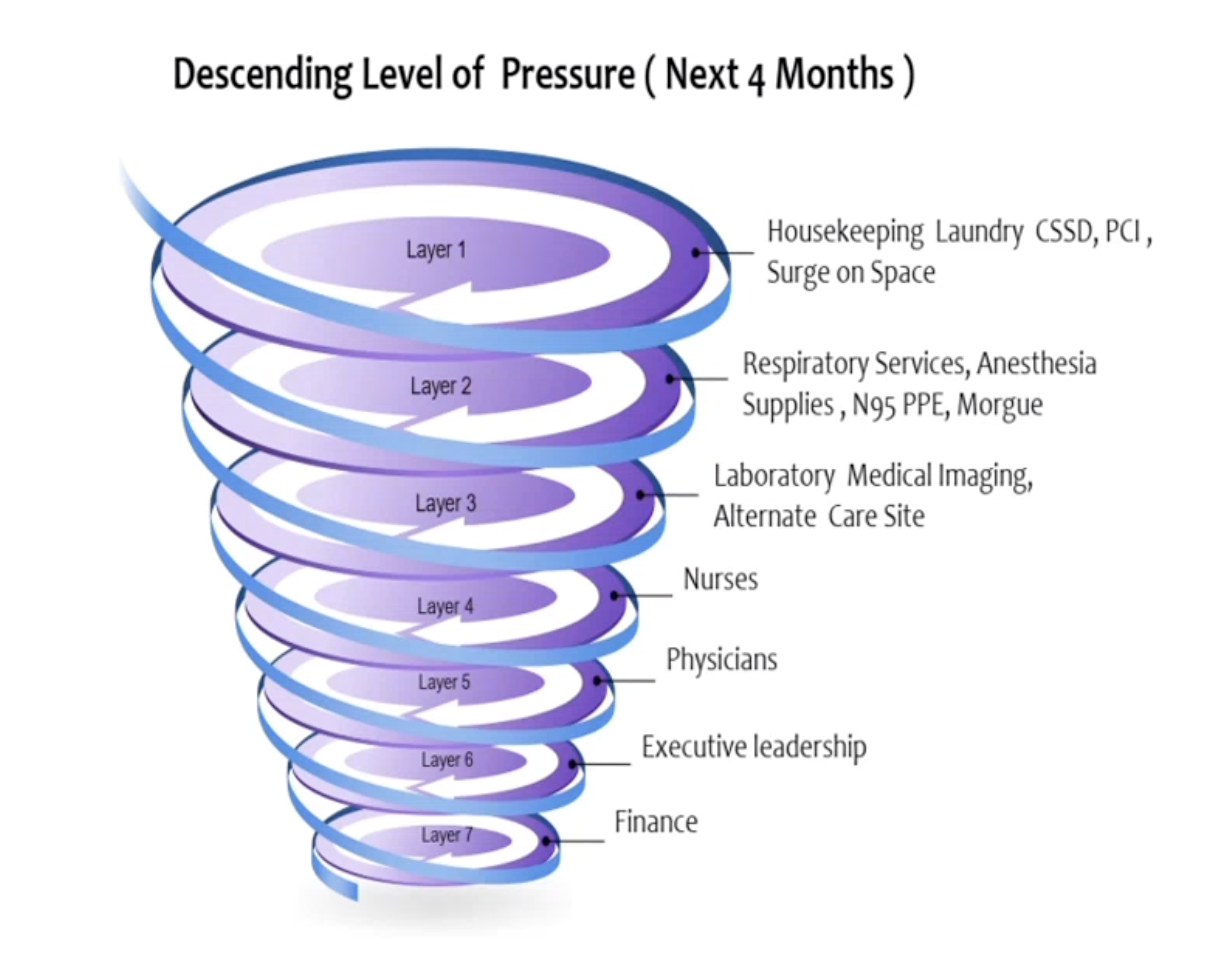
She further added that more than labelling hospitals as COVID-19 or non-COVID-19 it is important to unfold the complexities through an integrated approach. “We really need to integrate the approaches between healthcare facilities and public health systems,” she concluded.
9.55am
Good morning from Day 5 of Omnia Health Live, the final day! We're now minutes away from the first session. The coffee is ready. We are ready.
Thursday 25 June 2020
9.30pm
That’s us signing off for today! We look forward to welcoming you tomorrow for the final day of Omnia Health Live and bring you insights on healthcare investments, latest technology, among other hot topics.
9.22pm
And finally, if you missed it earlier, USCIPP provided a comprehensive insight into how post-COVID-19 medical travel might look, taking into account historical contexts and key factors shaping travel. Barriers to adopting technology were also named, taking into account air travel restrictions, and recommended strategies were offered. It was a fascinating presentation.
While pre-COVID US international medical travel was strong - 60 percent of USCIPP members reported volume increases year-on-year - the future is “complex”. Three possible scenarios were identified (by the University of Minnesota) for future COVID-19 cases in the US, while different US states will ultimately behave differently: a second wave; more stable control; and local flare-ups with peaks and valleys.
USCIPP took historical trajectories, including disaster recovery, Kondratiev waves and cycles of violence to provide a multifaceted historical context into 2020, which the data points to as an “unusual” year.
To get a sense of what might happen to medical travel after the current economic setback, USCIPP looked to two specific historic events in particular: 9/11 and the Financial Crisis.
After 9/11 overall tourist volumes took nearly 10 years to recover, but medical travel was much slower to recover. Conversely, travel volumes recovered more quickly after the “Great Recession” of 2008-09 - both travel trajectories (overall and medical) had begun to recover after 2011.
USCIPP provided an interpretation of these trends, and used this as a basis to forecast post-COVID 19 medical travel. In short, recovery is expected to be “challenging”.
The present economic crisis may have a lesser impact on inbound medical travel once regional economies begin to recover. The other COVID-19 implication is that consumer confidence about the US as a travel destination and visa restrictions are likely to have a bigger impact.
USCIPP highlighted many factors on how recovery might be shaped, both on demand and supply sides. The demand side factors were long and varied: air travel, cruise travel, vaccine availability, travel restrictions and more. Supply side included COVID-19 related hospital debt, hospital downsizing, and improved expertise for telehealth.
With air travel not feasible, technology is left to facilitate access to care - but there are barriers to using technology. These were identified in cultural, technical and legal areas - for instance providers having to accept the shift to healthcare services that are telemediated, US hospitals are using different platforms to deliver cross-border medicine, and legal concerns.
Diversification strategies going forward include collaborations across international borders and keeping international partners engaged - examples of international healthcare collaborations were shared on subsequent slides.
9:00pm
The last session for the day ‘Disinfection, sanitization and sterilization: concepts with which we will live from now on’ reviewed technological innovations in substances and cleaning methods that eradicate viruses, bacteria and germs.
Brian Reynolds, President of IAHCSMM 2020 said that due to COVID-19 hospitals have to reprocess instruments they wouldn’t normally just to make sure the immediate needs of both the patient and the staff are being met. “It’s been a big adjustment; we want to make sure this is temporary and once things are normal, we want to go back to our stringent processes.”
While Jason Unger, Director, Surgical Services and Anaesthesia Institute, Cleveland Clinic Abu Dhabi asked the important question of how can hospitals mitigate the chances of contamination in the first place? Some ways that this can be achieved is by giving patients options for virtual visits, sanitise everything in the facility at frequent intervals and even design hospitals in a way that can eliminate viruses in the first instance.
One of the other panellists, Patty Olinger, Executive Director, Global Biorisk Advisory Council, Division of ISSAWe, stressed that patient-centred care is of utmost importance, but if there are no healthcare providers, how can that care be offered. “It is important to ensure that there is adequate PPE and ensure manufacturers and healthcare organisations protect healthcare workers. Healthcare workers should put on their PPE before jumping into the thick of things! Also, it is essential for the operators of technologically-advanced sterilisation devices to be trained on what needs to be accomplished.”
7:45pm
It is a well-established fact that the beginning of the COVID-19 pandemic was followed by a health supply crisis. The pandemic changed everything by the minute and there were uncertainties about demand, scarcity of supplies, prices going up every hour, supply chain disruptions, etc.
As part of the 'The future of health supplies: production and distribution' discussion this evening, Juarez Miranda, Procurement General Manager, UHG, Brazil, said: “But every day we learnt from what was happening and reinvented ourselves very quickly.”
He gave the example of warehousing capacities of hospitals that usually don’t have big spaces for storage of materials and drugs. However, due to the pandemic, there was a need to store additional inventories and to secure supplies. “Therefore, we worked quickly towards global servicing in order to secure supplies,” he explained. “We also developed new business models with logistics operators in order to have capacities and capabilities to store and distribute products to all our hospitals.”
He stressed that post-COVID-19 countries need to focus on localisation and the healthcare industry needs to look at developing alternate sources and shouldn't rely on a single source for its manufacturing needs.
6:45pm
At the ‘Innov8 Talks - Healthcare Start-ups and Entrepreneurs Panel Discussion’, some of the most exciting global start-ups shared their experiences before, during and what plans they have post-COVID-19.
For instance, Ellington West, CEO & Co-Founder, Sonavi Labs, said that it initially took time to adjust to the new normal and it was difficult to connect with patients and healthcare workers. She said: “But we have learnt to operate and are coming together and supporting clinicians, which has been both challenging and inspiring. It has been such an awakening in a lot of ways. Our challenge is continuing this collaboration effectively.”
Paul Swinckels, CCO at LifeSense-Group, stressed that today, fewer people are going to the GP and there has been an increase in the use of telemedicine applications. “In Germany, previously there were just 1,000 GPs working with telemedicine, now there are 100,000 doctors working on it,” he highlighted.
While Ahmad Al-Kabbany, the founder of VRapeutic, said that COVID-19 has limitations that has significant opportunities. “There has been an urgency to deliver remote care. But COVID-19 was faster than all of us! This was in our product development plan, but the virus accelerated it. It completely updated our priorities.
“Moreover, innovation can help create new business or revenue stream. For us, COVID-19 was a pivot. We serve children with special needs at private clinics, therapy centres etc. However, due to the pandemic, we realised there was a communication gap between therapists and parents. This enabled us to innovate and we were among the five winners of a hackathon in Dubai, where we showcased our solution that helps connects therapists with parents effectively.”
3.58pm
Dr Rafael Grossman believes that healthcare is dysfunctional - and that technology can help fix this. Through using tools like Google Glass, he is better able to connect with the patient and ensure that they have a safer experience. At this point the first sci-fi reference came in ““We had head mounted displays in the Terminator”. Dr Grossman is also a prolific user of another medium for connecting with patients: online, that include social networks, a website and blog.
In his talk on how digital health and spatial computing can make surgery more accessible and affordable for all, he went on to cover areas that included VR, Augmented Reality (AR), Extended Reality (XR) and spatial computing. VR learning is better, he suggested, because of its higher retention rate. As an example of its application, he said a friend provided students with Google Cardboard, a product from 2015, so that they could travel inside the operating theatre.
Anima Res meanwhile offers an XR experience through 3D rendering, allowing surgeons to improve on how they operate on patients and allowing better outcomes through increased precision. One example shared by Dr Grossman was one of a human heart, hovering in the air like an alien being, allowing for any number of virtual interactions. “Imagine a patient looking at a lesion or abnormality; imagine a provider learning how to do a surgery.”
Tools such as Proximie allow expert specialists to guide surgeons with less expertise through facilitating a virtual connection. An expert surgeon based remotely, perhaps in a different part of the world altogether, can move their hand in a way that is manifested on the other end on top of a superimposed rendering, thus guiding the surgery. It’s a mix of two realities. What is especially exciting is that it’s a technology that doesn’t require 4G connectivity, and therefore it can be used in countries where 3G is the norm.
Other technologies introduced by the Venezuelan surgeon were also eye-catching - literally in the case of a contact lens with embedded circuitry, enabling AR projection in front of the wearer’s vision. Dr Grossman compared VNTANA (word derived from the Spanish for “window”, as you may have guessed) to Star Trek-stye teleportation. But while Star Trek beamed Scotty up, VNTANA can generate an approximation only, through creating a holographic display of individuals meeting.
3:15pm
This afternoon’s panel, ‘Availability and safety of blood supply during the pandemic of COVID-19’ shed light on how blood services all over the world have faced shortages since the beginning of the pandemic. The major concern of all blood services during this time has been the safety of donors and employees.
Panellist Dr Naima Oumeziane, medical director of Abu Dhabi blood bank/Sheikh Khalifa Medical City, Abu Dhabi, shared that the Emirate has been working hard to ensure the safety of all parties involved in the process. Some of the challenges have been the cancellation of blood drives due to COVID-19 restrictions on gatherings.
“The health authority has asked us now to call the donors and make appointments,” she said. “But the donors had anxiety about catching an infection while coming to the blood donation centres. Educating them is very important and the WHO has stated that we need to explain all the measures that are being taken to protect them.”
Some precautions that were taken included telling the donors to inform the blood bank if they had been in contact with a COVID-19 patient or if they have any symptoms, not to present themselves for blood donation. Donors were also told to call the blood bank back in case they have any symptoms in the 28 days after blood donation so that plasma can be recalled or disposed of since it has a long expiration period.
“Today, blood inventories have increased and we are able to go back to elective surgeries that had been stopped for four to six weeks and can support any hospital and patient,” she added.
3.00pm
That was a spirited talk by Dr Rafael Grossman of Google Glass fame, who drew parallels between the world of science fiction (The Terminator, Minority Report, Star Trek, and at least one other celluloid classic) and the emerging health tech of today! Notes to come...
1:00pm
The Global Burden of Disease report in 2017 showed that more than 56 million people had died from different kinds of diseases and back then there was no COVID-19. Today, more than 480,000 people have died of COVID-19. Dr Abulelah Hawsawi, Assistant Director General at the Central Board for Accreditation of Healthcare Institutions (CBAHI), Saudi Arabia, said that healthcare systems globally need to keep in mind that all the diseases that were there before will not go away and a measured approach is required to tackle these.
Speaking at the ‘New frontiers and innovations in Patient safety’ panel, he stressed that it is important to look at how we can address the safety of COVID-19 patients as well as that of other patients. “I was a COVID-19 patient myself back in March and was admitted for four days and have seen some of the challenges first-hand,” he shared. “There is a fear among health workers about contracting the disease that could result in delayed responsiveness and potentially put patients at harm’s way.”
He explained that non-COVID-19 patients are also facing a number of difficulties, having to do with the access to healthcare systems. Many patients are afraid to get into healthcare facilities as they are afraid of contracting the virus and many hospitals are finding themselves turning patients away. That challenge with access could result into many errors of omission in non-COVID-19 patients.
While Brenda Kubheka, Managing Director, Ethics and Clinical Risk Lead, South Africa, said that the safety of health professionals is important for the safety of patients in order to offer safe care. “If the safety of a healthcare worker is compromised, they basically become a biological hazard,” she said.
There are a number of elements that need to be looked at in a holistic way when it comes to healthcare workers, added Dr Mike Durkin, Senior Advisor, Patient Safety Policy & Leadership, Institute of Global Health Innovation, UK. “Their physical, mental, behavioural and social health needs to be focused on. Our responses to safety reporting has started to drift away and we have noticed that in our normal routine methodologies for incident reporting, we are seeing less reports within systems as well as nationally. Our performance indicators are also drifting.”
The moderator, Dr Michael Ramsay, Chief of Service, Department of Anesthesiology & Pain Management, Baylor University Medical Center, Dallas, U.S., highlighted that in Dallas, there was a 46 per cent reduction in people coming in who needed healthcare and did not seek it because they were fearful of coming into hospitals treating COVID-19 patients. Of those, 11 per cent suffered serious harm and there were significant amount of injuries to patients that could have been avoided. “We are now starting to address these concerns with telemedicine and virtual visits,” he said.
12.45pm
The four authors of a book, Voice Technology in Healhcare, partnered in a conversation earlier about voice technology's potential in enhancing provider and patient experiences. Among the observations shared in the discussion, led by Harry Pappas, founder & CEO of the Intelligent Health Association, were:
- companies and researchers are looking at being able to diagnose COVID-19 through voice. Hotspots could be identified through intonations
- the personalisation of the healthcare journey is going to change
- voice's benefits can be summarised as Versatile; Omnipresent; Innate; Contextual; Efficient (hence VOICE)
- voice assistants can take on a virtual companionship role and having a voice device at home can overcome health barriers. For example a senior citizen who might be alone in lockdown may ask to play Beethoven's 5th, or the voice system can serve to remind on appointments and prescriptions
- with any new technology however there will be apprehensions and abuses (intelligent mirrors could be listening for example)
10:48am
At this morning’s CME-accredited session ‘Enabling effective infection control across the Arab Gulf Region', speaker Wael Elamin, Consultant Clinical Microbiologist and Infection Control Doctor, Dubai, compared a pandemic with a play consisting of four acts.
The first act revolves around “progressive revelation”, where members of a community begin to acknowledge an increasing number of cases and or/deaths resulting from the spread of a contagious disease.
Act two – “managing randomness” – involves the society creating an intellectual framework within which the epidemic’s “dismaying arbitrariness” can be understood.
The third act is “negotiating public response.” Once an epidemic is recognised, the public typically demands that collective action of some kind be taken.
While the fourth act – “subsidence and retrospection” – is the most vexing phase of an epidemic, especially for those involved in public health management.
He added that epidemics often end as ambiguously as they appear and end “not with a bang, but a whimper.”
10.36am
Here's an interview we recorded earlier in the week with Sally Thompson, our Head of Conferences, to hear her thoughts on Omnia Health Live (no music, no exciting intro and outro, just raw words):
9.41am
Good morning from Day 4 of Omnia Health Live! How are you all feeling? The first session is due to commence shortly, on "Enabling effective infection control across the Arab Gulf region".
Wednesday 24 June 2020
9:00pm
The concluding session of Omnia Health Live Day 3 focused on the impact of data fragmentation in health institutions and in-patient care and how important it is to be able to answer quickly to an emergency and critical scenario.
Panellist Venkat Pydimarri, a Forbes Technology Council Member and AHIP IT Edn Board member, said that COVID-19 has shattered the belief that only clinical data defines how people are healthy. It has shown that the definition of health data itself is not anymore just about medical records. It is potentially all of the data that is surrounding the patient, such as clinical, financial etc. He said that in this fast converging and uniting world, anything that is done is going to be fragmented. Therefore, there is a lot of scope for further unification of data.
One of the other panellists, Atif Al Braiki, Chief Executive Officer, Abu Dhabi Health Data Service, said that data sharing is usually done for claims and reimbursement purposes between the payers and the providers. But between the different providers, previously in the UAE, there wasn’t a lot of data sharing for care coordination purposes. That was one of the drivers for the government of UAE to initiate the Malaffi, a Health Information Exchange (HIE) platform.
Juan Arellano, a CEO from Mexico concluded by saying: “Take it easy, we are all aiming for big data but first let's start with small data. Let’s start getting value out of something just to get started. We need to have a long-term strategy in case another pandemic comes our way.”
Join us tomorrow again to follow all the interesting highlights from Day 4 of Omnia Health Live! We will be discussing infection control, patient safety, medical travel and more.
7:30pm
Today’s keynote speaker, Dr Eric Eskioglu, executive vice president & chief medical officer for Novant Health in the U.S., started his presentation by exclaiming that COVID-19 has transformed what healthcare systems were not able to do in 10 years in just two months! As a result of this, healthcare delivery has evolved and patients have embraced telemedicine today rather than visiting brick and mortar facilities and exposing themselves to the virus.
He said: “We used to receive 150 telemedicine consults a year and now we get 6,000 a day! The use of AI will further develop telemedicine and enable healthcare workers to screen the calls and provide care to those that need it the most.”
Talking about industry trends, he stressed that accelerated burnout in healthcare providers is expected and this might lead to an acceleration of retirement. He added that this is again where AI will help healthcare out by being “assistive intelligence” and help the younger generation of physicians and increase efficiency in healthcare.
Dr Eskigolu stressed that the mental effects of COVID-19 will be here to stay for both patients as well as providers. “As physicians, we feel the pain every day,” he said. “Mental health issues will be soaring and there will be a great demand for it. There are not enough mental health workers and this again is where telemedicine and AI will play a key role. Everyone regardless of background should get access, as healthcare is the social fabric that binds us all and we have to make sure nobody is left behind.”
7.06pm
Blockchain is not a technology we hear too much about in healthcare, relative to AI for example, but consider this: a public blockchain such as Ethereum could have prevented the USD 9 billion Theranos fraud, according to Edward Bukstel, who spoke earlier on blockchain's potential to establish stronger transparency and security.
He explained that blockchain will be helpful in determining when information is authoritative, highlighting the problem of fake news and data - at one point mentioning "people talking about drinking disinfectant". He offered another example: he had his temperature checked en route to Dubai in February (Bukstel spoke at Medlab Middle East), but while surveillance is a good thing, there is potential for abuse.
There is a major emerging opportunity for blockchain to play a key role: the IoT medical devices market, espected to grow to USD 125 billion. Bukstel envisions a time when several medical devices are attached to an individual patient, to track blood oxygen, glucose monitoring and heart rate, for example.
Bukstel further outlined the following scenarios for blockchain's appication:
- Blockchain verification - first and foremost for patient identity, but also for verifying physician, specimen, laboratory and reagent identities.
- Blockchain powered AI surveillance in a laboratory context
- Beyond publisher paywalls
5.47pm
We're now roughly 15 minutes away from Edward Bukstel's talk on "Blockchain's role in COVID-19 response and recovery". We interviewed him recently on the arrival of telemedicine's tipping point.
5:00pm
The demand for blood and blood products is higher than supply, therefore, this calls for increased efforts in recruiting and retaining voluntary unpaid blood donors.
As part of the CME-accredited ‘Blood donor recruitment and retention strategies’ session, Dr Justina Kordai Ansah, Chief Executive Officer, National Blood Service Ghana; Expert Member for Transfusion Safety, WHO; Regional Director for African Region, ISBT; Chairperson, ISBT Working Party Blood Supply Management; Accra, Ghana, discussed some challenges faced in meeting blood demand globally.
These include ageing populations, iron depletion in regular blood donors, lack of systems and resources to support blood donor recruitment, and myths and misperceptions about blood donation, such as people thinking blood donation causes impotence or asking why they should give blood to an unknown person, etc.
She highlighted some innovative retention methods of blood donation that should be employed the world over. These include employing effective communication methods to provide education and information on blood donation, increasing mobile blood donation sessions in shopping malls, offices, etc., sending reminders to existing donors about their next appointment, telling donors when their blood has been transfused, ensuring a positive blood donation experience and making donors feel like heroes who have contributed positively to the society, among others.
4.32pm
Leading radiologists came together in an earlier session to share updates on imaging in COVID-19, with focus areas that included triage with imaging, portable ultrasound, and standardising reporting for chest CTs. The panel discussion was hosted by Prof Dr Michael Fuchsjaeger, Professor of Radiology and Chairman of the Department of Radiology at the Medical University Graz.
Updates were provided from Russia, Germany and Washington State in the US. All speakers began on an optimistic note, stating that their respective countries (or federal state, in the case of the US) were emerging strongly from the COVID-19 pandemic and seeing a return to normal life.
On imaging, Prof Dr Mahmud Mossa-Basha said that CT scans were performed when needed (there was no need for heavy use of imaging) in Washington, while according to Prof Dr Hans-Ulrich Kauczor in Germany CT scans were conducted on worsening patients, as well as on asymptomatic patients with negative test results. In Moscow, Prof Dr Valentin Sinitsyn, chief of the radiology department in the Federal Centre of Medicine and Rehabilitation, said the preference was to use CT instead of ultrasound; the Russian capital also created a network of up to 60 centres with CT machines, prescribed for patients who received medical attention at home.
On the use of AI, there was some skepticism.
Prof Dr Hans-Ulrich said that AI radiology software can always go wrong with low or intermediate prevalence of COVID in the population and that human expertise should be used for a differential diagnosis. He added that AI would be a great help in a second wave or another pandemic if tested on a broad differential diagnostic range of infectious lung diseases and produces good results.
Prof Dr Mahmud Mossa-Basha commented that while they have not implemented AI for COVID-19 in Washington state, vendors are asking for COVID-19 cases to develop an AI algorithm. In Moscow, Prof Dr Valentin Sinitsyn stated that AI is being used for the follow-up of patients but conceded that they were not true AI programs.
2.04pm
Here's an article that may interest you based on Monday's "Evaluating the transformation of Latin America's healthcare system after the COVID-19 pandemic" talk, authored by María José Ramírez/Grupo Expansión. It's a good write-up, while in Spanish (we'll have a translation ready soon, but you could probably use Google Translate for now).
1.39pm
If you missed it earlier, speakers in a session moderated by Dr Girdhar Gyani, Director General, Association of Healthcare Providers in India, discussed gaps in the healthcare system, how to manage asymptomatic patients, home care, and transformation in COVID-19 times, among other topics.
Perspectives were brought from India, Malaysia, Oman and Zambia, with the following insights shared, among many:
- Datuk Dr Kulijt Singh, President of the Association of Private Hospitals in Malaysia stated that the Southeast Asian country managed the crisis well - government hospitals did so without the involvement of the private sector, but there were worries over inadequate facilities. He highlighted the need for quick conversion into ICUs. While still very cautious in Malaysia - no one has escaped the COVID-19 screening process - financially things are picking up and he hopes for medical tourism to continue with the resumption of travel
- Dr Qasem Al-Salmi, Director General and CEO of the Royal Hospital in Muscat said that they were lucky in Oman: hospitals had sufficient flexibility to convert beds into ICUs. He nonetheless stressed the need for complementary healthcare; public health is an essential component of any health system. Like Malaysia, there is rigorous screening, with patients first offered questionnaires before any testing. On home care he said that many patients can be evaluated without physical examination; they don’t need to go to the hospital
- Dr Mohamed El Sahili, CEO at SF Group, brought up a challenge more specific to Zambia: the country is landlocked, and the supply chain was disrupted. The capacity of its healthcare system simply isn’t up to scale in terms of ICU and respiratory beds. On home care he highlighted trust and liability as a challenge, specifically how can a patient be made accountable for prescriptions given, such as receiving oxygen therapy at home?
In closing the discussion, all were agreed on the need to build resilience in systems to accommodate future challenges, and ensure that there is public-private integration. Dr Kuljit warned that COVID-19 wasn’t the worse in mortality, and there could be a bigger threat to come. COVID-19 had left an ominous mark: “If you couldn’t learn the last time, I will teach you.”
01:15pm
At the ‘Women's health care in the era of COVID-19’, Prof Marian Knight, Professor of Maternal and Child Population Health, National Perinatal Epidemiology Unit, Consultant in Public Health with Public Health England, Oxford, UK, discussed a recently published report about women who were admitted to hospitals with confirmed SARS-CoV-2 in pregnancy in the first part of April.
The report highlighted that the portion of pregnant women who died was similar to that of women of reproductive age who were also admitted to the hospital with SARS-CoV-2.
There were reportedly a number of women who had to be delivered pre-term to improve their respiratory situation and so of the babies. A quarter of babies were born pre-term. A relatively small proportion of babies were born very pre-term.
She said: “A lot of people were asking if the virus can be transmitted to babies. And the data we had from a national study showed that a small number of babies had subsequent positive tests. But only about 2 per cent had an early positive test. So, it looks like transmission occurring neonatally is quite uncommon.”
11:07am
At the ‘Validating testing during a novel pandemic’ CME-accredited session, American Hospital’s Dr Aaron Han reviewed overarching challenges in COVID-19 test validations and shared potential solutions.
He said that Serology tests will help play an important role in documenting vaccine efficacy. In some settings, NGS and sequencing will offer key assistance. “We will be embarking on more personalised treatment in the coming months. It is important for epidemiology and this information will offer guidance for travel, as countries start emerging from lockdowns,” he said.
9.35am
Good morning on Day 3 of Omnia Health Live! We’re approaching the midway point of the week’s activities.
Coming up we have a “Health providers panel on delivery system transformation” which will include Dr Kuljit Singh, whom you might remember from our interview, followed by a clinical session on "validating testing during a novel pandemic". Much to meditate on, and on that note we also have an introduction to meditation, led by Ben Veechai, Vice President of Marketing and Corporate Communications - Asia at Informa Markets.
Tuesday 23 June 2020
09:00pm
Today's concluding session put the spotlight on ‘Telemedicine and remote care’ with panellists discussing how patients and health professionals are dealing with the new perspectives on telemedicine, which has become an integral part of the new normal.
Rui Duarte Brandão, a CEO and Co-Founder from Brazil said: “With telemedicine, today you can enhance the patient journey, provide access, and with smartphones you can have a lot of data points and use that to personalise a patient’s journey.”
While Frans Hermes, a Managing Director from the Netherlands commented that there is an important duty today to use technology to make healthcare accessible to anybody. The systems can be designed to assist at an early stage, where it is possible to diagnose a disease earlier on or even help patients with chronic diseases manage their condition. At the same time, there is also a need to look at the business model.
He said: “If you go through existing channels, officially, everyone says technology is great, but before COVID-19 nobody really did it. But the pandemic has shown us the importance of such systems. If you could let people have access to this service for a minimal cost instead of them opting for expensive insurance schemes, that would be a big step forward for many countries.”
That’s a wrap for today! Join us tomorrow for another power-packed day where we cover topics right from women’s healthcare and medical imaging to blockchain's role in COVID-19.
7.52pm
There were interesting observations expressed earlier on promoting healthy living and wellbeing in COVID-19 times in a discussion moderated by Gareth Presch, founder and CEO, World Health Innovation Summit Platform for Sustainable Development. Again, much to dig into (too much to include on this page) that merits further attention, but the discussion had a strong people dimension that touched on areas of behavioural science:
- Michelle Ashen, Founder & CEO of Africans United, commented that there will be more nurse driven primary healthcare initiatives across society in Africa, and that mental health will play a big part in its resilience and ability to recover. She remarked it’s a major turning point as Africans.
- Mark Nichols, Head of Strategic Initiatives MENA Region, Senior Gulf Advisor, revealed that he’s never seen all sides of the market come together like now with COVID - governments, agencies, healthcare enterprises, and people - and that it’s a significant opportunity. He added that all are seeing potential in sustainable investments (he used the example of Saudi investment in India and China).
- Dr Paul Barach, Clinical Professor & Patient Safety Committee Member, raised the point that in order for pandemic efforts to work, people need to own their responsibility - there’s only so much governments can do. He pointed to the example of Taiwan, a nation of 28 million people, which identified scarce items and developed an app for these, thus avoiding panic buying and earning people's compliance. He explained that if people can access toilet paper, their trust can be earned on social distancing. Through giving up power and establishing transparency, it's possible to secure people's cooperation - and so Sustainable Development Goals can deliver opportuities, but only if government language and processes are altered.
- In a similar vein, Dr Barach mentioned that a deep discussion is required about privacy and transparency - to what extent do we trust governments with our data, in order to ensure that our societies are safe?
- Dr Manuela Boyle, external expert, Expert Advisor SDG 3, emphasised the need to foster e-health literacy, commenting that telehealth has changed much around the world because of COVID-19, becoming a fast-tracked reality.
7:45pm
Today’s keynote speaker, Dr Jim Merlino, Chief Clinical Transformation Officer, Cleveland Clinic, stressed that the task of healthcare leaders is first to deliver safe, high-quality care to people. Speaking at the ‘Transformation during a global pandemic’ session he highlighted other aspects that need to be given importance such as the fact that the care delivered needs to be centred on patients and families.
“We also have to evolve our cultures, particularly around working better together and developing high-performing teams," he said. “Moreover, we certainly have to control costs and provide greater access for people around the world to get the care that they need.”
But due to COVID-19, Dr Merlino said that Cleveland Clinic had a slight shift in its focus and realised that the organisation needed to double down and keep caregivers safe and healthy, otherwise it wouldn’t be able to deliver on its mission.
He said: “This included improving safety and quality surveillance, so quality and safety metrics that were being reviewed once a month were now being reviewed twice a week. The idea was to detect signals that could highlight if there was any drift in our performance. We also created caregiver support programmes to make their personal and professional lives easier.
“I am proud to say that while Cleveland Clinic had over 400 caregivers infected with the virus, not one of them faced an infection from taking care of a COVID-19 patient! This is a statement of the hard work we put into keeping our caregivers safe."
He closed the talk by quoting former U.S. President, the late John F. Kennedy: “…In a crisis, be aware of the danger – but recognise the opportunity.” Dr Merlino concluded: “One of the things I am most proud of at Cleveland Clinic is that not only did we do the work to keep people and caregivers safe but how we used this an opportunity to learn to make us better.”
5:50pm
Almost 2/3rd people globally with diabetes are not monitoring their condition according to recommendations, highlighted renowned diabetician, Dr Jonathan Rosenblum. Speaking at the ‘Breakthrough technologies for diabetes and its complications’ session presented by Evia Medical Technologies, the doctor shed light on some innovative technologies set to revolutionise diabetes care.
The first innovation is called EGM, a non-invasive glucose monitoring device that measures physiological changes in the earlobe tissue. It evaluates glucose by evaluating three independent readings using three different technologies: ultrasound, electromagnetic and thermal. It combines this with a unique proprietary algorithm, displaying reliable glucose result.
The EGM clips on the earlobe. Using ultrasound, glucose is evaluated by measurement of the sound velocity through tissue; thermal – glucose is evaluated through changes in HT characteristics when energy is supplied to tissue; electromagnetic – glucose is evaluated by changes in tissue impedance. Over 99 per cent of the EGM results are reportedly within the clinically accepted zone of the Consensus Error Grid for type 2 diabetes patients.
The second innovation is Sozo, which was originally designed for wound care therapy. In a recently published paper, it was shown that after only 8 treatments, more than 50 per cent of the Diabetic Foot ulcers responded positively to the device and resulted in wound closure.
5:00pm
Robots are becoming commonplace in healthcare today, even more so during the pandemic, as they don’t cough or get ill! The session 'Using conversational AI methods for human-robot interaction in healthcare' highlighted how today robots are being built that can handle multi-user conversations in lots of different scenarios, one of those being elderly care. This is interesting for a variety of reasons as robots can assist and amplify human efforts in different care tasks.

Oliver Lemon, Professor of Computer Science at Heriot-Watt University, Edinburgh shared that Herriot-Watt’s Alana system has been designed to deliver health-related information and support via conversational AI, during the COVID-19 pandemic. Some of its important features are that it can detect myths and misinformation and offers mental health advice. It only outputs validated sources of information such as from the WHO.
4.09pm
Experts from The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute (OSUCCC – James) convened minutes ago for a webinar covering work in cancer treatment, and insights into what the future holds for cancer research (in areas that include immuno-oncology, cancer engineering, haematology, radiation oncology and digital pathology). More to follow...
3:00pm
As part of ‘The use of stem cells and PRP in orthopaedic surgery’ CME-accredited session, panellists discussed the challenges when it comes to regenerative medicine and the acceptance of orthobiologics in surgery.
Professor Nicola Maffulli, Consultant Orthopaedic Surgeon and Honorary Professor for Sports and Exercise Medicine at the Queen Mary University of London explained that while people are talking about personalised medicine, it is important to understand that there will be some people who will respond to a given therapy and some will not. This applies to everything including surgery.
“The best surgeon is not the one who does the operation well, but the one who knows how to select patients well. Up to now for orthobiologics (spanning stem cells, PRP etc.), we have not had any good ways of determining who will benefit from a given intervention and more research is required,” he said.
1.46pm
Dr. Tedros Adhanom Ghebreyesus, Director General of the WHO, is a healthcare leader who has become a household name in recent months owing to his public role in the global pandemic response. In his video address early this afternoon at Omnia Health Live, he communicated the following points (edited) that underlined the need to build a better world with the global healthcare industry playing a strategic role in its development:
We’re now 6 months into the defining health crisis of our times
More than 8.4 million cases have been reported to the WHO
More than 150,000 have lost their lives.
The situation is improving in some countries, globally it’s worsening.
For the last 2 weeks, more than 100,000 cases have been reported daily
It’s so much more than a health crisis. Millions have lost their jobs. The global economy is headed for the sharpest contraction since the Great Depression. The political, economic and social effect of the pandemic will be felt for years to come
The health industry has never been more important
The pandemic has told us that health is not a luxury item, but a human right and the foundation for social and economic development
We learned the hard way that health is central to everything
The health industry will play an essential role in creating a healthier, safer and fairer world we all want
We should be all in this together.
12.22pm
We've just followed the Advance Health webinar - much to unpack, too much for a live blog, but in essence the expert panel convened by Dubai Science Park's Marwan Abdulaziz Janahi, shared diverse perspectives on areas such as advancing telemedicine and data privacy, with fascinating references to WhatsApp, YouTube, Boeing 777 air travel, the Spanish Flu and gazelles (yes, really) included. A great, relaxed conversation. Insights on accelerating digital health included the following - but do view the full discussion:
- Dr Mohammad Al Redha, Director, Project Management Office, Health Informations & Smart Health in Dubai commented that the availability of data made it possible to take timely action and control the situation. He however stressed the need for greater integration for a more coordinated action across government - the more systems integration the better
- Christine Arakelian, CEO of Global Healthcare Integrators, emphasied the point that the advancement of digital health isn’t a technology question (since Google would otherwise be running healthcare); what’s currently missing is the ability to have more cohesive patient data sets, that would then be of interest to multiple stakeholders
- Dr Louise Schaper, CEO of Australasian Institute of Digital Health (AIDH), suggested that there is a need to upscale the workforce in digital health (training on why to use data). Digital health is ultimately about putting patients first. Dr Schaper hopes it would be "politically unpopular" to wind back to how things were before the pandemic
- Alex Butler, co-founder of Foundry3 and UK based, questioned whether technology could continued to be adopted after the pandemic
Here's a 'sneak peek' of the discussion, courtesy of a Twitter user:
11.58am
Much happening at the moment, and taking a moment to check reactions on social media. Here's someone who enjoyed yesterday's Tom Lawry session, sharing a highly tweetable statistic:
10:50am
This morning’s CME Accredited panel ‘World-class quality management within multidisciplinary health services’ touched upon some of the biggest challenges in Quality Management today.
Panellist Dr Karen Luxford shed light on a number of key factors in relation to quality management framework. These included having clear corporate governance and leaders placing an emphasis on safety and quality. Also, making sure that policies and processes are in place and aligned throughout the organisation. Moreover, engaging clinicians in clinical governance particularly within multi-disciplinary settings and making sure they are engaged in key decision-making.
10.30am
Omnia Health Live's Advance Health webinar is now just half an hour away. But meanwhile, we invite you take a look at our newly published Q&A with Dubai Science Park managing director Marwan Abdulaziz Janahi, who is chairing the webinar, on the importance of digital privacy as healthcare goes digital amid the COVID-19 pandemic. And to get a flavour of what’s to come, here’s an earlier Advance Health webinar on the importance of mental wellbeing during the outbreak.
9.10am
Good morning from Dubai! We're now into Day 2 of Omnia Health Live. We have the WHO's Dr Tedros speaking later, following a panel discussion on "world-class quality management within multidisciplinary health services" and an Advance Health webinar on digital healthcare. There's also another yoga session to look forward to in a short while, the intriguingly titled (and sci-fi sounding) "core ladder sequence".
Monday 22 June 2020
8.28pm
Did you see Tom Lawry's presentation earlier? If not, read on...
Microsoft’s National AI Director started his talk with an encouraging message on Omnia Health Live, virtual platforms and networking from his home office (thanks, Tom!). His presentation was on AI and the Creative Destruction of Healthcare, in which he talked about AI transformation in healthcare and what the future AI health leader looks like.
But first, let’s start with one of his more interesting slides. It’s the most intriguing chart of the day - a correlation between per capita cheese consumption and the number of people who died by becoming tangled in their bedsheets (something to think about the next time you reach for the fridge last thing at night). It’s a spurious claim - a classic case of correlation versus causation. Through machine learning many different correlations or patterns are possible, said Lawry, but our ability to use these rests on the wisdom, experience and common sense of human workers. AI will aid whatever work is done in the care process by knowledge workers.
He shared interesting examples of AI's recent value in healthcare that came about within weeks of COVID-19’s emergence. Early on, a COVID-19 Open Research Data Set (CORD-19) was created - studies, research, articles were brought together and indexed for researchers and scientists using Microsoft’s knowledge extraction tool. Microsoft also put together a coronavirus health bot adopted by organisations such as CDC that fielded millions of consumers queries and offloaded work that would have be done by humans.
In addition, AI is used to strength telehealth, and there’s a huge body of work being done looking at an intelligent return to work approach, and its use in predicting future outbreaks.
As for the "creative destruction", it's a reference to Eric Topol's use of the term (in a 2013 book) and AI's role in transforming processes and work to increase value. AI's emergence will lead to the rise of intelligent health systems. Correspondingly, a new type of leadership is required - the AI health leader.
It's exciting, and revolutionary (Lawry concluded with a Jefferson quote, "Every generation needs a revolution" - which seems fitting for today's times). Look out for an article on this.
7:50pm
What is the impact of chronic conditions in different health systems today and how is each place dealing with the patients? What are the health systems learning about risk stratification, early diagnosis and patient care?
Some of these questions were answered at the ‘Chronic Conditions - Redesigning the Health System’ session this evening.
Eduardo Jorgensen, CEO at Medicsen, explained that some of the main problems revolve around solving the outpatient problem and shifting care models to become more patient-centric rather than hospital-centric.
“We found that there are some problems when it comes to this approach,” he said. “The first one being around regulations that prevent hospitals and even the doctors themselves to be in these kinds of solutions because there is a lack of trust. The second point is around funding. Hospitals are huge machines that are used to certain models, so when you try to enter alternative models, the value of return on investment is really hard to secure. I believe that until governments start paying for that we are going to see some struggle in this area.”
6:45pm
One of healthcare’s biggest challenges today is that to what degree do health systems have the digital capacity to engage every consumer and every citizen globally, when and where needed to help them stay healthy. This includes helping prevent people from getting infected by COVID-19 or managing other chronic conditions. This is the heart of where digital health ecosystems play an important role.
At the ‘Digital Maturity: Improving Outcomes, Building Health Systems’ Resilience’ session presented by HIMSS, Dr. Anne Snowdon, Professor of Strategy and Entrepreneurship, Academic Chair of the World Health Innovation Network (WIN) and Scientific Director and CEO of SCAN Health, explained how a mature health ecosystem looks like.
She said such a system needs to focus on population health but also have the ability to drill down to individual health and personalise care delivery. “You can do that only if you have a highly interoperable digital/connected data network that tracks population and individual outcomes so that teams can identify care models,” she said.
According to Tim Kelsey, senior vice president of Analytics International at HIMSS, some of the drivers of digital health are safety and quality and to really empower people to make choices more effectively for themselves, in partnership with their clinicians.
“Another important driver is that without digital data, without the ability to record and share data, which allow for analysis, we can’t support the development of new medicines or treatments or implement technologies that already exist, for instance, genomics,” he stressed. “A really important focus for governments, beyond the immediate pressures of COVID-19, is just long-term investing in a service that is going to encourage the development of new medicines.”
6.23pm
Still with us? Tom Lawry, National Director for AI at Microsoft, is soon to give a talk on AI and the Creative Destruction of Healthcare - you may remember him from his guest article The future is not what is used to be. Excited? You should be.
5:40pm
Women make up almost 80 per cent of healthcare workers, and it has been evidenced that women-led nations had a better response when it came to dealing with COVID-19. This afternoon’s session on ‘Female leadership: Forging a new era of effective healthcare’ saw female leaders give some powerful insights.
Andrea McGonigle, National Managing Director, Health & Life Sciences Industry, Microsoft shared that when you think of a household, the women is the CEO and from that perspective, by being a decision-maker in healthcare, women bring diversity of thought to the table.
While Clare Omatseye, a CEO, President from Nigeria said: “Women play a major role in all aspects of the healthcare industry. We see more women rising to the top. However, even more women are required in leadership roles. You have much more robust decision-making when a woman in on board. There is no glass ceiling, the sky is the limit for us! I tell a lot of young women that you can have it all, but maybe not at the same time, so you need to clearly define what success means to you.”
On the other hand, Dr Manuela Boyle, Expert Advisor SDG 3, shared that women have to deal with challenges such as gender stereotypes, family responsibilities, networking opportunities etc., at the workplace.
“Healthcare is an industry where women represent 65 per cent of the workforce. However, they are underrepresented,” she said. “For instance, in Australia and New Zealand, they make up only 13 per cent of managerial roles.”
She explained that leadership has three dimensions – ability, affinity and integrity. While ability and integrity are self-explanatory, affinity is different because it involves caring for another person and having empathy. “This is where men and women have different ways of approaching the situation. Leadership means to inspire and communicate effectively, and women are able to do that very well.”
To conclude, Simone Rudolph Shortt, Director, PeonyCo said: “Women need to have confidence in themselves and to walk the walk!”
5.32pm
Earlier this afternoon, pathologist Dr James Walter Snyder, Director of Microbiology and Infectious Disease Molecular Diagnostics at the University of Louisville Hospital, Louisville, US, shared his experience on how his lab handled massive COVID-19 testings and measures for when the pandemic slows down.
Describing how in December he saw that a new virus had emerged in China, and believing then that there was a chance of it spreading to the US (like H1N1 and SARS), he stressed the importance of playing “what if” - or having a 5 year plan, and being prepared.
Dr Snyder highlighted issues such as turnaround time when outsourcing to commercial laboratories (the plan was to test on a 24/7 basis, including weekends, and initially they could only test 4-5 per day), and the need for better communication with technologists, who had become stressed.
On POC testing, he doesn’t believe it’s ready for “prime time”, saying that its sensitivity is very low. Testing generally will be ongoing, he said, but whether it recurs at the same level “no one knows”.
3.52pm
Phew! Professor Neil Greenberg packed in a lot of information in his talk on maintaining the mental health needs of healthcare workers, but it was a mental health talk with a difference. Prof Greenberg is an academic psychiatrist with a military background - he served in the UK Armed Forces for 23 years - and so his presentation was peppered with fascinating references from Afghanistan to former US Secretary of State General Marshall (perhaps better known for the Marshall Plan).
He warned that, while COVID-19 cases continue to come down, mental health needs remain high. Members of the general population at risk included BAME and low income groups; people previously infected with COVID-19, owing to neurological consequences with a psychological component still not understood; people grieving COVID-19 victims, especially “complicated” grief cases; occupational groups like healthcare workers; and previous or current mental health sufferers.
He added that half a million people are experiencing mental health problems owing to the current economic downturn in the UK.
In the UK, risk factors among healthcare workers included those who were younger and/or junior; parents of dependent children; a longer quarantine; a lack of practical support; and stigma.
Prof Greenberg went on to share what does - and doesn’t work - from a mental health management perspective, and included powerful insights and data from military contexts and former disease cases. Strategies included Trauma risk management (TRiM), which he colourfully described as "not a pink and fluffy approach" with incense, but a way of actively monitoring staff to see how they’re doing.
Well worth a watch (or listen).
3.30pm
At 4pm, Dr James Snyder and Dr Robert Sautter will highlight important considerations to be kept in mind for starting up testing during a dangerous pandemic in a short period of time to help treat patients and keep populations safe. Register for the session here.
2.22pm
We're rapidly approaching mid-afternoon, and it's been a day of "play" as well as work. If you took part in the Yoga-lates Core Fusion earlier, send us a picture of your core fusion-inspired yoga moves - we'll publish the best (do take care, however)!: [email protected] or [email protected]
2.13pm
Did anyone catch the earlier panel discussion on cancer care delivery challenges and solutions in the pandemic?
The talk presented very interesting contrasts. While India is in a “very bad situation”, or a crisis within a crisis, in the words of Dr Abhishek Shankar, Dr Kiran Turaga - based in Chicago - described how city and state responded effectively to lockdown and that the recovery phase was underway, currently at 80 percent of normal cancer for patients after stopping surgeries in March.
Dr Cary Adams meanwhile considered himself “lucky to be in Switzerland”, describing it as the safest place for COVID in the world. The Central European country now sees 20 new cases per day. He however warned of complicated cancer cases in the months ahead. His words were powerful: “cancer doesn’t disappear for 3 months just because COVID is around”.
He also highlighted a major concern: cancer organisations are facing difficult financial circumstances with a consequence for future cancer control, believing the impact will be felt over the next 24 months or longer.
In the UAE, Dr Humaid Al-Shamsi attributed declining COVID-19 cases to a strong emphasis on testing (“I myself have been tested eight times”) - 45,000 tests have been carried out daily. Asymptomatic patients who are on chemotherapy continue to be screened on a regular basis.
Looking ahead, there was some optimism. Dr Adams stated that COVID-19 presented the best opportunity ever to make the case for (cancer) prevention - everyone stayed indoors and followed the rules, while governments for the first time recognised that health impacted the bottom line. Governments now realise that investing in healthcare is a good idea.
Dr Humaid Al-Shamsi pointed to the strengths of the UAE’s healthcare system (“the way to go in the future”) and Dr Turaga highlighted the benefits of innovation, through sharing examples such as data sharing and rise of telemedicine (charges approved by the government).
Here's what a Twitter user made of it:
01:20pm
At the ‘Clinical Value of Spike Protein Antibody in the Diagnosis of SARS-CoV-2 Infection’ session, Dr Moner Ragas, Regional Scientific Marketing Manager (EMEA), Beckman Coulter Diagnostics, said that not all tests detecting IgG antibodies are the same.
“The Beckman Coulter Access IgG assay targets the RBD of the spikes (S) protein as it is critical for viral entry, and antibodies targeting this domain of SARS-CoV-2 have been shown to be neutralising in laboratory studies and may confer immunity,” he said.
Furthermore, the majority of the vaccine production platforms for SARS-CoV-2 are using S protein as the main target.
Additionally, serology or antibody testing may be a vital tool for determining who has developed an immune response to SARS-CoV-2, thus allowing to better quantify the number of cases of COVID-19 including those that may be asymptomatic or have recovered.
12:15pm
As part of the ‘Hemoglobin, Coagulation & Oxygenation in COVID-19 Patients’ session presented by Masimo, Dr Mark Robinson, Consultant Haemotologist at Cambridge University, explains the damage COVID-19 can cause to different organs through the below illustration.
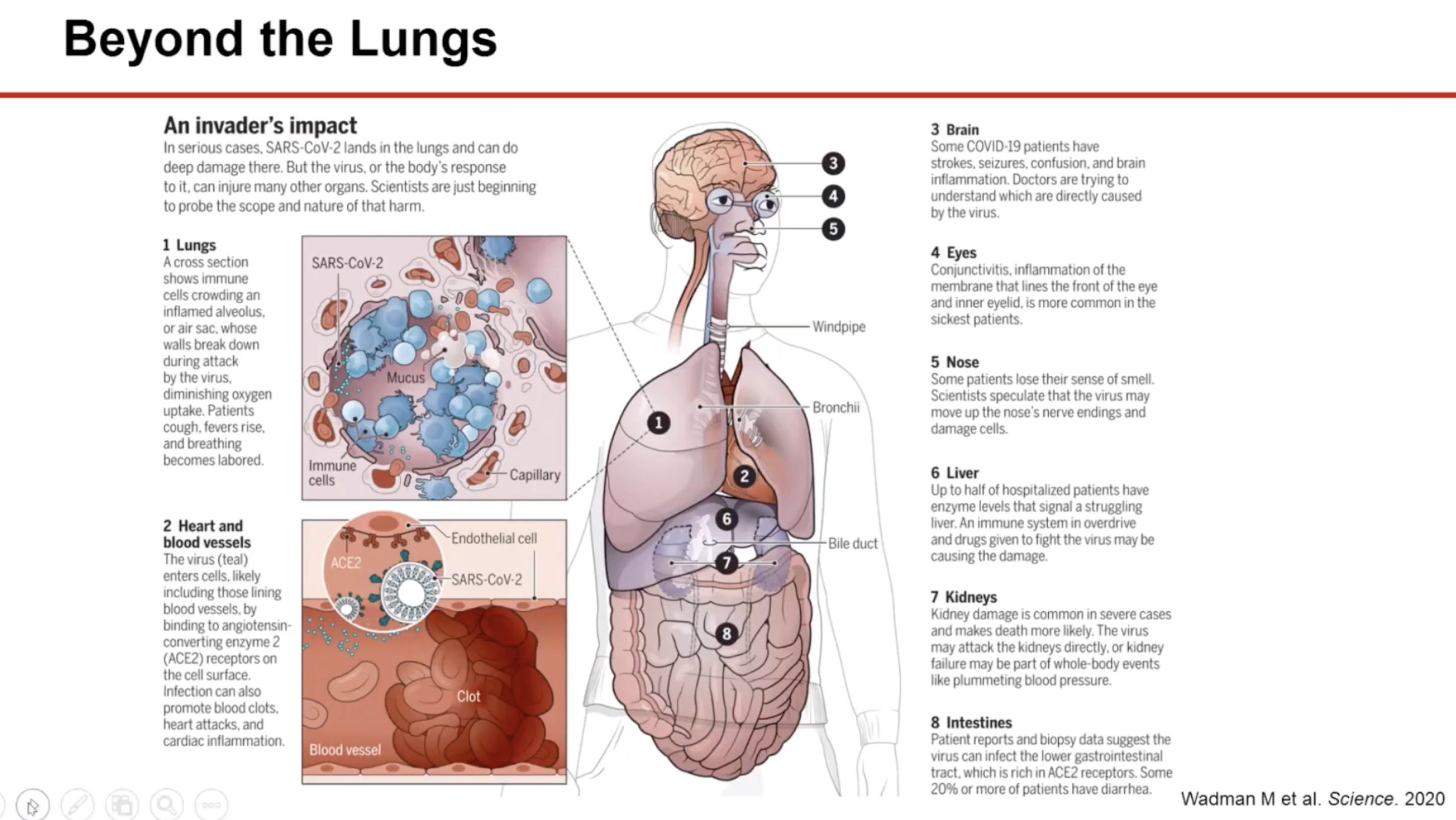
11.52am
If you also missed the earlier session on COVID-19's impact on medtech, moderated by Rami Rajab, chairman of Mecomed, here's a quick overview. Rajab opened by sharing an update on how Mecomed cooperated with governments during COVID-19:
- sharing a list of direct contacts for essential COVID-19 equipment with authorities;
- publishing an open letter to governments to ease regulatory requirements during the outbreak;
- publishing compliance guidance document for members and their partners during the outbreak;
- and joining the Global Medical Technology Alliance in an open letter to G20 governments
The panel, made up of executive names in medical manufacturing, was asked to share challenges and expectations in the new COVID-19 environment. Shared challenges included the following, and they included strong engagement elements:
- communication - communicating with employees, distributors, partners and healthcare professionals to ensure they were engaged
- ensuring the health, wellbeing and motivation of employees. Working from home was challenging - and empathy and finding innovative solutions were key to making it work
- business continuity and post-pandemic recovery. There is the complication of geographies moving at different speeds/recovering at different times - and organisations will need to be better prepared for any future outbreak
In terms of expectations, business recovery and a return to normal will be "slow", but there will be opportunities to explore new business models, innovations and collaborations.
Concluding the session, among other considerations Rajab highlighted the industry's social obligation (to society), and that time and money can be saved through innovation that results in faster surgeries and better recoveries. While thanking the industry, he reserved special gratitude for healthcare providers in their pandemic.
He ended with an apt point and something to dwell on in these chronically uncertain times: "We always need a plan C".
(You might also be interested in our Mecomed story from Arab Health.)
11:50am
In an earlier session today, Cath Murphy PhD, a registered nurse currently with the Australian College of Perioperative Nurses (ACORN), stressed that while we believe Personal Protective Equipment (PPE) will provide safety and reduce the risk of harm, the caveat is that not all risks are equal.
“Sometimes particular infectious diseases require much higher levels of PPE or have much more easy transmission rate, so the risks are not equal. Another important point to note is that human behaviour comes into this whole notion of PPE. The way that healthcare workers use PPE varies enormously. The way PPE is used reflects a clinician’s ability to align their assessment to the potential risk and make the appropriate choice,” she highlighted.
11.10am
The Mecomed-chaired panel dicussion on the Impact of COVID-19 on the MedTech industry in the MEA region has just concluded. A few common trends emerged in the participants' responses. Notes to follow...
10:15am
The CME-accredited 'Lab management during the COVID-19 pandemic' session is now underway, featuring heads of laboratories from Asia, Europe and the Middle East. Panellists are discussing the extended role of laboratory diagnostics in managing COVID-19, and providing an overview of the current situation in their countries and management lessons.
For instance, Dr. Januario Veloso, Consultant Hematopathologist, Department of Pathology, UP College of Medicine, the Philippines, shared that his hospital built an in-house SARS-COV-2 PCR testing facility. He said: "Initially we thought the goal would be 300 tests per hour but it later increased to 1,500 tests."
While Nattiya Hirankarn, Chair of Clinical Microbiology Department of Microbiology, Faculty of Medicine, Thailand, highlighted: "In Thailand, during March and April, we had to look after patients not only in our hospital but also from hospitals in nearby locations. However, at the moment, the situation is getting much better and we haven't had any new cases for more than two weeks now."
Dr Joris Delanghe, Clinical Chemistry Laboratory, Belgium, added: “Belgium has been hit severely by COVID-19. The cases were maximum in April but now hospitals and clinical laboratories are coming to pre-COVID-19 activity levels. For the labs, it means business as usual, apart from the fact that they now have to strictly follow social distancing, systematic use of face masks and intensive hand hygiene.”
9.30am
While still on the subject of yoga and wellness, there will also be a session today on Staying safe & staying sane: Sustaining and maintaining the mental health needs of healthcare workers, delivered by Dr Atiya Mosam, Public Health Medicine Specialist, Researcher and Executive Board Member, and Prof Neil Greenberg, Professor of Defence Mental Health.
Prof Greenberg has posted the following on Twitter (would be interesting to hear his thoughts on social media and mental health - a conversation for another time):
9.14am
Coming up, we have three Omnia Health Live sessions beginning within the hour: Impact of low quality PPE on infection control in Australia and Lab management during the COVID-19 pandemic (both clinical sessions, CME accredited), and an industry talk - Presented by MECOMED: Impact of COVID-19 on the MedTech industry in the MEA region.
There will be several other talks with a COVID-19 theme today - fortunately we also have a virtual yoga session later in the day to put our minds at ease a little (delivered virtually; you will have to do it for real).
8.52am
Informa plc CEO Lord Stephen Carter's video address has just ended. If you didn't catch it, here's what he said (edited for brevity):
Hello and a very warm welcome to Omnia Health Live.
I’m Stephen Carter, group chief executive of Informa, the business behind Omnia Health Live. We are thrilled to be producing and introducing this event to the healthcare community.
Many of you watching and particiapting may well know us, or some of our other brands or products, and have been part of the international healthcare communities we’ve tried to serve or support.
We’ve been thrilled to bring our internal healthcare community inside Informa together to produce and curate Omnia Health Live.
It is a 100% digital event, like many of the things that many of us are doing.
It will allow open access to subject areas to professional interest areas to personal passion areas.
It will allow to allow practitioners and professionals to accrue professional accreditation in professional areas of interest.
Not surprisingly it will provide access to shared learning, especially around discoveries and experiences the healthcare communites are having in relation to COVID-19 discovery, diagnostics and treatment approaches around the world.
There is a whole range of technology applications emebdded in Omnia Health Live. You can create subgroups, create your own schedule, you can matchmake with professional peers, or you can follow the schedule of the hundreds of individuals speakers and panels that pique your interest.
Along the way, there will be specific practical applications, whether product demonstrations or professional accreditations.
We’ve tried to design and curate this to make this three dimensional, or as as three dimensional a virtual event can be.
We’d be delighted to host this physically, but we’d be more delighted to do this physically and accompanied by the richness and longevity embedded during the week long digital connection.
On the other side of COVID-19 we will be doing more of these things, the physical and digital together.
I hope you find lots of value, and hope you’ve had as much as fun as the team inside Informa has had in producing and curating it.
Thank you for your participation and for our professional contribution at this critical time in the world where healthcare innovation, policy and professionals are right in the centre stage of all our lives.
Enjoy Omnia Health Live, and do take care.
8.34am
A warm welcome to you from Dubai! We'll be starting Omnia Health Live coverage shortly. Coffee ready, but it's not the usual takeaway cup this time - it is, of course, a virtual event. Today's proceedings will be commenced with an opening address by Informa chief Lord Stephen Carter.
Sunday 21 June 2020
Happy Father's Day to all the dads out there, and if you have a spare 25 minutes please give our new Patient Talk podcast listen - the first two episodes are focused on men's health (physical and mental), with insights and advice shared by leading Dubai physicians.
But we're thrilled to share that everyday is a celebration this week. Yes, Omnia Health Live is upon us, the virtual healthcare event taking place over five days, bringing together the global healthcare community during these challenging times.
As previously with Arab Health, we will live blog the week through sharing quotes, snippets, speeches and anything else that comes to mind, so don't forget to bookmark this page. You can also follow and join the conversation through the hashtag #omniahealthlive.
To get things started, we're delighted to reveal an additional speaker to the lineup - and what an addition. Introducing Dr Tedros Adhanom Ghebreyesus, Director-General of the World Health Organisation (WHO), who has been rather active these past few months. Dr Tedros will be sharing a few words on Tuesday.
To further whet your appetite meanwhile, here are just a few stories you will find on this website that feature Omnia Health Live participants:
- The future is not what it used to be: how Ai can be a force for good in healthcare
- Evolving role of the laboratory
- Dr Kuljit Singh: public private partnerships are the way forward post-pandemic
- How to be prepared for a pandemic
- Reinventing healthcare delivery
- Telemedicine's tipping point has arrived, says blockchain guru
- Department of Health’s Malaffi: Connected information facilitating smarter care
- Sonavi Labs AI stethoscope to help detect COVID-19

