A painful hip, without a direct traumatic origin, is a frequent complaint in children, whilst young children most often present with a limp. Next to clinical presentation, the differential diagnosis can be narrowed down by the age at presentation.
Awareness of the fact that children can present with knee pain, due to hip pathology (referred pain) is important and vice versa, especially young children can have pathology in the knee, lower leg or foot.
Clinical presentation
Trauma
When a child presents with hip pain or a limp, parents are inclined to ask for a history of trauma. This can be misleading as children virtually always remember a history of some fall or minor trauma. Important is to directly relate the beginning of pain with the supposed trauma.
Fever
Next to hip pain, it is important to note feelings of general illness and fever, as bacterial arthritis is a surgical emergency. Furthermore, osteomyelitis can have normal radiological findings on conventional X-ray in the early stage of disease. In case of fever, blood examination is required.
Age
The most important factor in making an appropriate differential diagnosis is the age of the patient, as some diseases occur more often in certain age groups (Table 1).

Septic arthritis
Bacterial arthritis is usually caused by Staphylococcus aureus and can have a rapidly deteriorating course with destruction of the joint. On ultrasound there is joint effusion. Note that the echogenicity of the fluid is not of diagnostic value. The synovium may be thickened, but this is also a non-specific finding. Joint effusion and the clinical profile are the keystones for the diagnosis. Immediate aspiration and surgical debridement should be performed. Absence of joint effusion excludes septic arthritis.
Radiographs are not sensitive to joint effusion and are not helpful in the early diagnosis.
Osteomyelitis
Osteomyelitis is a relatively common severe condition in children. As in septic arthritis, Staphylococcus aureus is the most common pathogen. In suspected osteomyelitis, MRI is the imaging method of choice. In infants or young children in whom the location may be uncertain, bone scintigraphy can be useful.
Most radiographs will not show abnormalities in the early stages of the disease, but after 7-10 days osteolysis and periosteal reaction are seen.
In young children ( < 1.5 year) there are still vessels in the physis, so infection may easily spread to the epiphysis and joint. In older children the physis forms a natural border for spread of infection (Fig. 1). Ultrasound can be helpful in visualising subperiosteal abscess formation or fluid collections. MRI will also demonstrate the joint effusion and synovial thickening, but can also show damage to the bone and cartilage. On MRI osteomyelitis appears as an area of T2 increased signal in the metaphysis with enhancement and surrounding edema in the soft tissues, and occasionally a subperiosteal abscess. Brodie’s abscess is a subtype of subacute osteomyelitis, which is typically seen in children, with intraosseous abscess formation occurring usually in the metaphysis. As the abscess is encapsulated by a rim of granulation tissue, systemic symptoms such as fever and inflammatory markers may be absent.
Referred pain
Because young children may have difficulty communicating the problem, it may be necessary to image the entire extremity.
Under the age of four a relative common cause of a limp is the Toddler fracture, a spiral fracture of the tibia or fibula caused by stress on juvenile bone because of “excessive”walking.
A common cause in the foot is Köhler’s disease, an idiopathic osteonecrosis of navicular bone.
Trampoline fracture is typically located in the proximal tibia metaphysis and can be very subtle.

Figure 2. Toddler fracture of the distal tibia.
Non-accidental injury
Non-accidental injury is beyond the scope of this paper. For imaging protocols the guidelines of the Royal College of Radiologists is recommended.
Transient synovitis
Transient synovitis (coxitis fugax) is an aseptic inflammation of the hip, presumably of postviral aetiology. It is the most common cause of hip pain or a limp in children under the age of ten years.
Affected children are only mildly ill or have recently sustained a low-grade respiratory tract infection. The condition is self-limiting and treated with rest and if necessary analgesics.
Imaging is not strictly necessary, but an ultrasound is often requested to confirm the presence of a joint effusion. Radiography is only performed when there are other differential diagnostic considerations. The appearance of the effusion on ultrasound is not helpful for the differential diagnosis.
Always consider the possibility of septic arthritis in a sick child!

Figure 3. Anechogenic effusion in the hip (between markers).
Perthes disease
Perthes disease, also known as Legg-Calvé-Perthes disease, is an idiopathic avascular necrosis of the proximal femoral epiphysis. It occurs more commonly in boys, typically between 5 and 8 years of age, but may range from the ages 3-12. It can occur bilaterally, but it is usually asymmetric. Early radiographs may be normal or show subtle flattening of the femoral head (Fig.4). Sclerosis and subchondral fractures may develop, features best appreciated on the frog-leg lateral view.
Treatment is symptomatic. If disease progresses, fragmentation and collapse of the femoral head will occur and metaphyseal lucencies can be seen.
In the healing phase, Perthes disease can lead to a short, broad femoral head and collum, known as coxa magna deformity. The radiologic differential diagnosis of Perthes disease includes secondary avascular necrosis (due to underlying disease, or medicamentous). Meyer’s dysplasia and multiple epiphyseal dysplasia can have comparable radiological findings, but are mostly bilateral and symmetric, whilst Perthes disease is, if bilateral, mostly asymmetrical.
Slipped Capital Femoral Epiphysis
Slipped Capital Femoral Epiphysis (SCFE) or femoral epiphysiolysis is an idiopathic Salter-Harris type I fracture of the proximal femoral epiphysis. It occurs more commonly in boys and in obese children. The typical age at presentation is between 12-15 years. SCFE may occur bilaterally in up to one third of cases. As the epiphysis slips posteriorly, and to a lesser extent medially it is best appreciated on the frog-leg lateral view (Fig.5). SCFE is treated with surgical fixation to prevent further slip off. Avascular necrosis of the femoral epiphysis is a potential complication.
Avulsion injuries
Avulsion injuries of the pelvis are a frequent cause of hip pain in adolescents involved in sports. Because at this age the tendons are generally stronger than the apophyses, strong muscle contraction can result in apophyseal avulsion fractures (Fig.6). Avulsion injuries can be acute or chronic.

Figure 4. Frog-leg lateral view. Early phase of Perthes disease with subchondral fracture line.
Bone tumors and tumor-like lesions
There are many bone tumors and tumor-like lesions that may cause pain in the hip or upper leg. We will not discuss the various bone tumors.
Juvenile Idiopathic Arthritis
Juvenile Idiopathic Arthritis (JIA) is an autoimmune, noninfective, inflammatory joint disease of more than 6 weeks duration in children under 16 years of age. It is a clinical diagnosis and is currently divided into six different subtypes. Contrary to the adult population, cartilage loss and erosions are not a frequent finding in JIA. X-rays are usually negative early on in the disease. Typical findings in children in later stages of the disease may be a slightly larger epiphysis, or accelerated bone maturation. Ultrasound will show effusion, thickened synovium and sometimes hyperemia.

Figure 5. Lauenstein view with right (H) sided slipped capital epiphysis.
Normal variants
In order to avoid false positive results on X-ray imaging one should be aware of normal variants that may simulate disease. In newborn babies up to 6 months, a symmetric physiologic periostal reaction can be seen around the diaphysis of the long bones, probably due to rapid growth rate. This should not be mistaken for non-accidental injury. Osteochondral connections, like the ones of the pubic bones can be mistaken for an abnormality. Awareness of the various normal variants is useful and when in doubt consider examining the other side to compare.
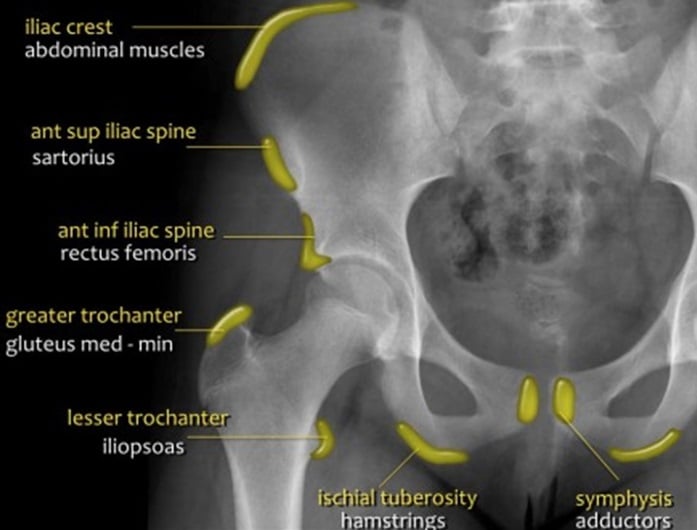
Figure 6. Sites of common avulsion injuries and muscle attachments.
Imaging modalities
As stated earlier several imaging techniques can be useful (Table 2). In children from 4 to 10 years old with symptoms for less than 5 days, and in the absence of high fever or elevated inflammatory markers - a wait-and-see policy is recommended. In these cases, the diagnosis is usually transient synovitis, which is a spontaneously resolving condition. In most cases osseous pathology can be excluded with a frog-leg (Lauenstein) view only. In case of suspected pathology on the frog-leg view, an additional AP radiograph should also be acquired for orthopedic and follow-up purposes. It is important to realize that in transient synovitis and early in the course of Perthes disease, juvenile idiopathic arthritis, osteomyelitis and septic arthritis, the initial radiographs are normal.

Lead Shielding
Gonadal shielding is dissuaded because of risk of masking important diagnostic information, a higher number of retakes and possible shielding of automatic exposure control chambers.
Conclusion
Hip pain and limping in children is a challenge for all clinicians. A practical approach is presented. Take good care of the sick child with fever and elevated inflammatory markers, as bacterial arthritis is a surgical emergency. A history of trauma can be misleading. Focus on the age of the patient in decision making for further radiological examinations. In case of persistent unexplained complaints consider MRI and especially in the young child, bone scintigraphy might be useful.

