Hospitals are arguably some of the most demanding and challenging buildings to design. They house a diverse range of specialist clinical services each with their own critical design, function and process requirements. With continuous advancements in research, technology, expectations, needs and policy, healthcare planning demands expertise to optimise performance and efficiency, in a challenging competitive market.
At the inception of each development project, the aspirations and vision are outlined. These initial objectives may be driven by service demand or infrastructure deficiency, but all healthcare projects have the one common goal of improving healthcare delivery.
The overall success of a project can be traced back to the time and effort invested at the early stages, when the strategic plan and brief is defined. Changes later on become progressively more expensive as the project develops and can lessen the integrated nature of the design. There is a tendency to rush this stage as it seems unproductive, but it is imperative that a strategic assessment of all influencing factors is carried out to ensure that the project vision is achieved in the most effective manner to optimise health and investment outcomes.
Emerging and strategic issues that influence a hospital’s service and infrastructure requirements range from: demographics and epidemiology; healthcare statistics; site conditions; regulatory criteria; technological opportunity; and financial feasibility. The healthcare planner is adept at gathering, organising and assessing available data in order to predict the current and future service demand and prioritise needs. For long lasting success, healthcare facilities need to be able to adapt to accommodate future changes in demand, expectations, care and technology.

Each healthcare project deserves a unique solution, developed to address the particular needs of the client and region. It takes knowledge and understanding of best practice in healthcare design across the globe to effectively adapt to diversity in socio-economic profile, resource or time constraints. While health inequality exists, experience and insight offer strategic opportunities for sensitive yet successful results in any market.
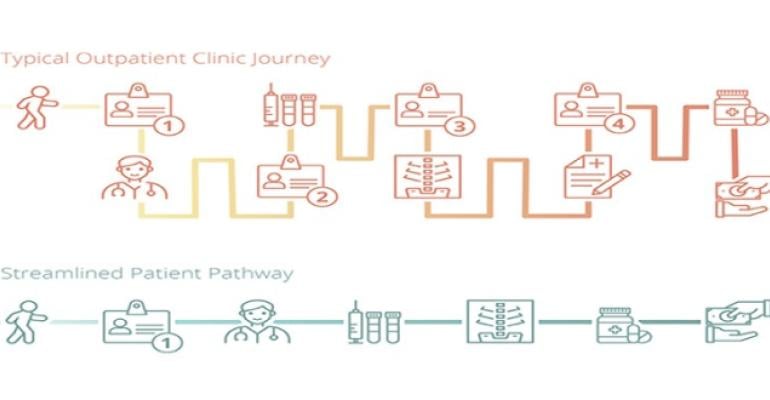
Before putting pen to paper on designs, the briefing process offers the greatest opportunity for the client and users to influence the design. The brief typically describes the scope, function, quality, timescale and cost of the project, but on a healthcare project, the briefing process additionally involves the definition of clinical design standards such as: operational capacity targets; operational principles; patient flow charts; configuration guidelines; and notable medical equipment. The brief is the highest level of control document throughout a construction project, therefore its completeness at the outset is fundamental to the efficient progress of the development.
Healthcare projects involve a multitude of stakeholders, often with disparate and conflicting views. Clinical professionals’ input, together with strong client leadership, is highly valuable in defining the service needs and functional requirements of each department, such as the workload and operational procedures. The healthcare planner acts as the nucleus of this process of knowledge sharing amongst stakeholders to reach the best solution for patient care delivery. This involves discussion of new models of care; evidence-based design; new technology and regulatory constraints. These aspects can have a significant impact on the sizing of departments, with for example, a shift from healing to prevention leading to larger diagnostic and treatment facilities and a reduction in bed numbers.
Before putting pen to paper on designs, the briefing process offers the greatest opportunity for the client and users to influence the design.
It is important to consider that clinical professionals may not have experience of construction projects and this drawn out process has significant demands on time for regular meetings, to initially inform the brief and latterly the designs. There tends to be a common difficulty in identifying the exact requirements and recording them in writing.
To progress on the basis of incomplete instructions leads to provisional decisions being made, that may have major implications later. The healthcare planner holds the experience to ask the right questions; the objectivity to identify real needs; the skills to overcome challenges; and the tools to establish an effective communication system, to manage the complex and dynamic web of information and requirements. This systematic approach eases pressure on the clinical, client and design teams and ensures that informed decisions are made on-time.
Beyond the briefing stage, the healthcare planner remains a valuable member of the design team, acting as a single point of contact for clinical queries from the architects, engineers and project managers involved in developing the project. The healthcare planner can assert the needs of the patient and clinicians, throughout design, coordination and construction process.
Embarking on the design of a hospital project should not be underestimated, as indicated by the extensive and specialised preparation works involved. The need to provide ever increasing quality, value-based healthcare in a competitive market demands healthcare planning expertise. The healthcare planner’s knowledge and understanding of service objectives; clinical processes and technical implications, drives the team towards opportunities to improve efficiency and advance the model of care. Through innovation, optimisation and flexibility in strategic planning, the healthcare planner can add value, reduce risk and maximise the lifespan of the development. Investing time in the pre-design stage pays dividends, not only in time and money, but furthermore in the fundamental objective of improving health outcomes.
Through innovation, optimisation and flexibility in strategic planning, the healthcare planner can add value, reduce risk and maximise the lifespan of the development.